Chapter Outline
- Developmental Abnormalities of Enamel
- • Amelogenesis Imperfecta
- • Environmental Enamel Hypoplasia
- • Nonspecific Abnormalities
- • Turner Hypoplasia
- • Molar Incisor Hypomineralization (MIH)
- • Dental Fluorosis
- Developmental Abnormalities of Dentine
- • Dentinogenesis Imperfecta
- • Dentine Dysplasia
- • Dentine Dysplasia Associated with Other Conditions
- Developmental Abnormalities of Enamel and Dentine
- • Syndromic Composite Abnormalities of Enamel and Dentine
- • Regional Odontodysplasia
- Developmental Abnormalities of Cementum
- Developmental Abnormalities of Number of Teeth
- • Hyperdontia
- • Hypodontia
- Developmental Abnormalities of Eruption of Teeth
- • Early Eruption Including Natal Teeth
- • Delayed or Failure of Eruption of Teeth
- Developmental Abnormalities Resulting in Early Loss of Teeth
- Developmental Abnormalities of Tooth Form and Size
- • Microdontia and Macrodontia
- • Dens Invaginatus
- • Dens Evaginatus and Enamel Pearls
- • Taurodontism
- • Gemination
- • Fusion
- • Concresence
- Basic Principles and Management of Patient with Developmental Anomalies of Teeth
- Acquired Abnormalities of Teeth
- • Attrition
- • Abrasion
- • Erosion
- • Abfraction
- Internal and External Root Resorption
- • Internal Root Resorption
- • External Root Resorption
- Tooth Discoloration and Staining
- • Intrinsic Discoloration
- • Extrinsic Staining
- • Internalized Staining
- Self-assessment Questions
INTRODUCTION
This chapter describes some of the main developmental and nondevelopmental abnormalities of teeth.
Developmental abnormalities of teeth can arise through either inherited mutations in genes involved in tooth development or exposure to environmental factors during the development of teeth, that disrupt or modify the development process. The genes involved in tooth development can be classified into two main groups: genes whose function is critical in tooth development but not other tissues and genes whose function is critical in development of many tissues, including teeth. Pathological mutations of the former result in nonsyndromic conditions in which there are only abnormalities of teeth. In contrast, mutations of the latter result in syndromic conditions in which the abnormalities of teeth are associated with a range of other phenotypic changes. There are numerous syndromic, single gene- or Mendelian disorders that present with abnormalities of teeth. For brevity, only some of the more common conditions are described below. Their systemic manifestations are not described in detail here but are readily available from Online Mendelian Inheritance in Man (OMIM).
The nondevelopmental abnormalities of teeth are those that arise through the action of the environment (e.g. mechanical wear, chemical erosion) on fully developed teeth. The description given below excludes an account on dental caries (see Chapter 2).
DEVELOPMENTAL ABNORMALITIES OF ENAMEL
Amelogenesis Imperfecta
Amelogenesis imperfecta is the term given for a group of genetically and phenotypically heterogeneous disorders affecting the enamel. These abnormalities can occur in isolation (nonsyndromic) or as part of a syndrome and generally, affect all teeth resulting in altered structure and appearance of the teeth. The reported prevalence of amelogenesis imperfecta varies between 1 in 700 and 1 in 14,000.
The abnormalities and the resultant clinical and histological appearances in amelogenesis imperfecta vary (Table 1.1, Figs 1.1 and 1.2).
The consequences of poorly formed or mineralized enamel are rapid breakdown, poor esthetics, predisposition to caries and thermal sensitivity. Management is focused on exclusion of any systemic features, preservation of tooth structure and improvement of esthetics by restorative care such as prosthetic crowns or plastic restorations, prevention of dental caries and maintenance of good oral hygiene, psychological well-being of the individual and genetic counseling.
Nonsyndromic Amelogenesis Imperfecta
A number of classifications of the amelogenesis imperfecta based either on morphology, mode of inheritance and/or genetic or biochemical defect have been proposed.
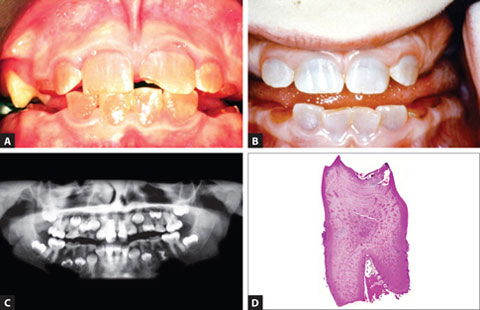
Figs 1.1A to D: (Courtesy: Professor I Mackie)
Amelogenesis imperfecta. (A) Hypoplastic-hypomineralized amelogenesis imperfecta with discolored, rough soft enamel with pits and ridges; (B) Hypomineralized amelogenesis imperfecta with discolored, rough soft enamel; (C) Hypomaturation type amelogenesis imperfecta with whitish patches; (D) Radiographic appearances of hypomineralized amelogenesis imperfecta showing poorly mineralized enamel
Figs 1.2A and B: (Courtesy: Dr K Hunter)
Amelogenesis imperfecta. (A) Ground sections showing hypoplastic amelogenesis imperfecta with thin irregular enamel; (B) Hypomineralized amelogenesis imperfecta with enamel of relatively normal thickness but with poor mineralization
4Classifications based just on morphology or modes of inheritance as primary discriminants are inadequate because of phenotypic and genetic heterogeneity and gene dose dependency of some of the traits resulting in different modes of inheritance. A classification based on molecular pathology provides a sound but possibly somewhat incomplete basis to consider this group of conditions.
Amelogenesis imperfecta can be inherited as X-linked or an autosomal recessive or dominant trait. A number of genes with pathogenic mutations have been identified in amelogenesis imperfecta. The genes, the resulting phenotypes and mode of inheritance are shown in Table 1.2. It is presently unclear whether or not all types of nonsyndromic amelogenesis imperfecta reported to date can be attributed to mutations in one of the genes listed in Table 1.2. At least one other type of amelogenesis imperfecta mapping to the distal part of the long arm of the X chromosome has been reported previously.
Mutations in AMELX result in a classical X-linked recessive trait with males fully expressing the phenotype whilst females show alternate banding of normal and affected enamel due to Lyonization. Mutations in ENAM can result in either dominant or recessive traits with either localized or generalized hypoplasia respectively suggesting dose-dependency of the trait.
Syndromic Amelogenesis Imperfecta
Amelogenesis imperfecta also occurs as part of several Mendelian conditions often with abnormalities of other ectodermal derived tissues. For example, in tricho-dento-osseous syndrome amelogenesis imperfecta is associated with taurodontism and other variable phenotypic changes including curly hair, bony sclerosis and brittle nails. In Jalili syndrome, amelogenesis imperfecta is associated with conrod dystrophy. Amelogenesis imperfecta is also seen in some syndromes with abnormalities of calcium metabolism or regulation such as nephrocalcinosis, vitamin D dependent- and independent-rickets. Abnormalities of enamel have also been reported in numerous other rare Mendelian disorders.
Environmental Enamel Hypoplasia
Environmental insults or disturbances during tooth development are associated with enamel defects. These can range from small area of opacity to larger areas of discoloration, pitting, grooves and involvement of the whole crown (Fig. 1.3A to C). Change may be distinctive or nonspecific. The timing of disturbance in development is indicated by the position of the defects on the crown and the teeth affected.
|
Figs 1.3A to C:
Environmental hypoplasia. (A) Enamel hypoplasia localized to one tooth; (B) Enamel hypoplasia of the permanent lower central incisors as result of trauma to deciduous lower central incisors at 18 months (Turner hypoplasia); (C) Enamel hypoplasia characterized by pits affecting upper central and lateral incisors
Thus, disturbances in utero present on deciduous teeth, disturbances in the first two years present on permanent anterior and first molar teeth, and disturbances in years 4 and 5 on canines, premolars and second molars.
A variable prevalence of enamel hypoplasia has been reported but most accounts suggest between 10 and 15 percent in the adult population. In a majority of cases this affects a single tooth, usually buccal surface of anterior teeth.
Nonspecific Abnormalities
A variety of environmental factors have been reported to be associated with enamel hypoplasia. These include low birth weight, viral infections, fever, prenatal or neonatal respiratory insufficiency/distress, malabsorption syndromes such as celiac disease, malnutrition, cytotoxic therapy, other drugs, metabolic disorders, parathyroid disorders.
Some specific types of environment-induced hypoplasia are also recognized and are described below.
Turner Hypoplasia
This is enamel hypoplasia of variable severity thought to be associated with periapical infection or trauma associated with preceding deciduous teeth (Fig. 1.3A to C). Hypoplasia associated with periapical infection is most commonly seen in permanent premolars whilst that due to trauma is more commonly seen in maxillary permanent incisors.
Molar Incisor Hypomineralization
This is defined as hypomineralization of variable severity associated with systemic factors and affecting one or more permanent first molars with or without incisors involvement. The reported prevalence of molar incisor hypomineralization (MIH) varies between 2.5 and 25 percent. The etiology is unknown but is thought to be associated with many of the factors described above including infections of upper aerodigestive tract, exanthamatous fevers and antibiotics. MIH presents as well delineated white, yellow or brown opacities usually on the buccal or occlusal surfaces. The lesions are asymmetrical in contrast to amelogenesis imperfecta and fluorosis. The teeth are prone to thermal sensitivity and caries. Management includes early diagnosis, remineralization, caries prevention, restorations, extractions if necessary and orthodontic care.
Dental Fluorosis
This is defined as developmental abnormality of enamel due to excessive fluoride exposure during tooth development. Excessive intake of fluoride anytime after birth up to the age of approximately 8 years can result in fluorosis with the severity, number and type of teeth involved determined by the dose, the period and the timing of exposure. The key sources of fluoride in this respect are fluoride in the water, supplements and dentrifices.6
Fluorosed enamel shows both maturation and mineralization defects with retention of amelogenin, increased porosity and subsurface hypomineralization.
The prevalence of fluorosis in the permanent teeth varies widely between and within countries and depends on factors such naturally occurring fluoride levels of the water supply, water fluoridation and other supplementation schemes. Some studies indicate that between approximately 10 and 20 percent of the population in areas with water fluoridation may have fluorosis that is of esthetic concern.
Clinically the appearances of fluorosis can vary depending on the severity of the fluorosis (Fig. 1.4). Mild changes consist of a few small white specks or streaks to larger opaque areas. More severe changes range from small stained pits to large confluent areas of pitting with prominent brown staining. The defects are symmetrical and diffuse, unlike changes associated with other environmental enamel defects.
DEVELOPMENTAL ABNORMALITIES OF DENTINE
Classically, inherited defects of dentine have been classified into two main broad groups: dentinogenesis imperfecta and dentine dysplasia (Table 1.3).
Fig. 1.4: (Courtesy: Dr Manil Fonseka). Management of fluorosis is focused on improving the esthetics. In mild and moderate fluorosis, combinations of microabrasion, bleaching and restorations will usually suffice. For severe fluorosis, prosthetic crowns may be necessary
Fluorosis. Teeth are chalky white in appearance with some teeth showing brown discoloration
Dentinogenesis Imperfecta
The prevalence of dentinogenesis imperfecta is thought to be between 1 in 6000 and 1 in 8000 whilst dentine dysplasia is much rarer with reported incidences of about 1 in 100,000.
Dentinogenesis imperfecta is further subdivided into three types: dentinogenesis imperfecta occurring with osteogenesis imperfecta (type I) or in isolation (type II and III).
|
7Dentine dysplasia is subdivided into two types based on phenotypic differences: type I or radicular and type II or coronal. However, it is now apparent that dentinogenesis imperfecta types II and III, and dentine dysplasia type II represent a spectrum of phenotypes resulting from mutations in the same gene (DSPP) encoding dentin sialophosphoprotein. Dentinogenesis imperfecta type I arises as part of osteogenesis imperfecta with mutations almost always (but not exclusively) in the two genes (COL1A1 and COL1A2) encoding collagen type 1. The genetic defect in dentine dysplasia type I has not been identified as yet.
The specific features of each these conditions are described below. The principle consequences of poorly formed dentine are discoloration of the teeth, shearing of enamel from the dentine, rapid breakdown of teeth, pulpal exposure, and pulpal and periapical infection, and early loss of teeth in association with poorly developed roots. Surprisingly, despite widespread exposure of dentine, thermal sensitivity is not a prominent feature because of dentinal sclerosis. The key principles in management are exclusion of systemic features such as osteogenesis imperfecta, preservation of teeth through protective restorations such as prosthetic crowns, prevention of dental caries and periodontal disease, and genetic counseling.
Nonsyndromic Dentinogenesis Imperfecta (Types II and III)
Dentinogenesis imperfecta is a term used to define defects of dentine affecting both primary and secondary dentition resulting in characteristic clinical, radiographic and histological appearances. These include blue-gray or brown opalescent teeth that show rapid and marked attrition after eruption (Fig. 1.5A and B). Radiographically, the teeth have bulbous crowns, narrow roots and pulp canals obliterated by pulp stones (1.5C). Histologically, the dentine is abnormal with areas of interglobular dentine, irregular and variably reduced number of tubules, and pulpal calcifications (1.5D). These characteristic changes are seen in dentinogenesis imperfecta type II.
In dentinogenesis imperfecta type III, instead of the pulpal obliteration, prominent pulpal enlargement due to hypotrophy of dentine is seen with consequent multiple pulpal exposures and apical infection. Radiographically, the teeth appear as ‘shell teeth’ and mandibular incisors often have apical radiolucent areas due to pulpal exposure and infection. Initially, this phenotype was thought to be limited to a dentinogenesis imperfecta occurring in a tri-racial population of Brandywine, Maryland, USA. However it is has been observed in unrelated families elsewhere and only seen in 2 percent of the Brandywine dentinogenesis imperfecta cohort suggesting this phenotype does not represent a distinct entity but is part of the variable expressivity of dentinogenesis imperfecta.
Syndromic Dentinogenesis Imperfecta
Dentinogenesis imperfecta associated with osteogenesis imperfecta (Type I)
Dentinogenesis imperfecta is most commonly observed as part of osteogenesis imperfecta and is classified as dentinogenesis imperfecta type I with features that are identical to nonsyndromic dentinogenesis imperfecta type II. It can occur in all types of osteogenesis imperfecta but is most commonly seen in types III and IV and only with missense mutations in either COL1A1 or COL1A2. Occasionally, dentinogenesis imperfecta may be the most penetrant feature of this condition and thus, it is important to seek relevant history and features of osteogenesis imperfecta in all cases of dentinogenesis imperfecta.
Dentinogenesis imperfecta associated with other conditions
Dentinogenesis imperfecta may be observed as part of other rare conditions with mutations in COL1A1 (Goldblatt syndrome) or COL1A2 (Ehlers Danlos syndrome type VII). It is also observed in other rare syndromes associated with mutations in other genes or for which the genes have yet to be identified.8
Figs 1.5A to D: (Courtesy for Figure 1.5C: Professor K Horner); (D) Histological section of decalcified tooth showing poorly formed dentine with irregular tubules and obliterated pulp chamber (Courtesy forFigure 15D: Dr K Hunter)
Dentinogenesis imperfecta. (A and B) Clinical appearances of opalescent teeth with rapid breakdown of the crowns; (C) Radiographic appearances showing bulbous crowns with short narrow roots with obliterated pulp chambers and root canals
Dentine Dysplasia
Dentine Dysplasia Type I
This is the rarest of inherited dentine disorders and is characterized by teeth with virtually normal crowns but abnormal root development hence the alternative name for this condition of radicular dentine dysplasia. Both deciduous and permanent dentitions are affected and clinically presents as mobility of teeth and early tooth loss. The condition is usually diagnosed by radiographic examination either as an incidental finding or following history of early tooth loss. The teeth have short, conical roots with either completely obliterated pulp chambers (deciduous teeth) or almost completely obliterated pulp chambers (permanent teeth). Histologically, teeth have normal enamel with an adjacent narrow zone of normal appearing dentine beyond which there are whorled masses of dysplastic tubular and atubular dentine (Fig. 1.6A and B). Apically, the whorled dentine masses are replaced by a less uniform arrangement of dysplastic dentine. Apical radiolucencies are also seen.
Dentine Dysplasia Type II
This condition is virtually identical to dentinogenesis imperfecta type II but largely only affects deciduous dentition (Fig. 1.7) with the permanent teeth either unaffected or having thistle shaped pulp chambers with multiple pulp stones. Thus, differential diagnosis of opalescent primary teeth should include dentine dysplasia (DD) type II in addition to DG.9
Figs 1.6A and B: (Courtesy: Dr K Hunter)
Dentine dysplasia type I. (A) Ground section; (B) Decalcified section; of an affected permanent incisor showing lack of root development, normal enamel with an adjacent zone of normal appearing dentine beyond which there are whorled masses of dysplastic tubular and atubular dentine partially obliterating the pulp chamber
Dentine Dysplasia Associated with Other Conditions
Dentine dysplasia is seen in association with other conditions including disorders of phosphate and/or calcium metabolism.
Fig. 1.7: (Courtesy: Professor M Dixon)
Dentine dysplasia type II. Deciduous teeth show discoloration and rapid breakdown of the crowns whilst the permanent dentition is unaffected
In familial hypophosphatemic vitamin D-resistant rickets, an X linked dominant condition, enlarged pulp chambers with prominent pulp horns, marked interglobular dentine and increased thickness of predentine (Fig. 1.8A and B) are seen in association with bone deformities, osteomalacia and growth retardation. The condition often presents with multiple periapical dental abscesses due to early exposure of the pulp horns in anterior teeth.
Figs 1.8A and B:
Familial hypophosphatemic vitamin D resistant rickets. (A) Decalcified section of a permanent molar showing abnormal dentine involving the whole tooth; (B) Higher magnification view; showing in detail the marked interglobular dentine and increased thickness of predentine
Dentine dysplasia with short bulbous roots, pulp stones and partial obliteration of the pulp cavity occurs in hyperphosphatemic tumoral calcinosis, an autosomal recessive disorder, characterized by progressive deposition of calcified masses in soft tissues.
DEVELOPMENTAL ABNORMALITIES OF ENAMEL AND DENTINE
Composite developmental abnormalities involving both enamel and dentine probably occur in many Mendelian syndromes but have not been defined adequately. They have been described in Mendelian disorders of calcium and phosphate metabolism, and collagen some of which are describe below. Non-syndromic composite abnormalities also occur in regional odontodysplasia, a nonhereditary segmental condition of unknown etiology.
Syndromic Composite Abnormalities of Enamel and Dentine
The X linked dominant condition familial hypophosphatemic vitamin D-resistant rickets characterized by enlarged pulp chambers with prominent pulp horns, marked interglobular dentine and increased thickness of predentine has been described above. Although the changes in dentine are the most prominent features of this condition, the enamel also displays variable hypoplasia.
In vitamin D dependent rickets types I and II, the teeth show similar changes in dentine including increased size of pulp chambers, variable mineralization, interglobular dentine, increased thickness of predentine and variably sized tubules. However, the changes in enamel are more prominent and characterized by hypoplastic/hypomineralized yellow–brown enamel. In addition, the teeth do not appear to have the predisposition to early pulpal exposure and development of multiple periapical abscesses seen in familial hypophosphatemic vitamin D-resistant rickets.
Ehlers-Danlos syndrome (EDS) is a genetically heterogeneous connective tissue disorder resulting from mutation of genes encoding some types of collagen or proteins necessary for collagen assembly. There are six types of EDS showing either autosomal dominant or recessive modes of inheritance. There is broad spectrum of clinical features ranging from mild to severe that include joint hyperextensibility, skin laxity (1.9A), and tissue and organ fragility leading to aneurysms, bowel rupture or retinal detachment.
Figs 1.9A and B: Ehlers-Danlos syndrome. (A) Skin laxity; (B) Periapical radiograph of teeth showing roots with pulp stones and dilacerations
Figs 1.10A and B: (Courtesy forFigure 10A: Professor K Horner)
Regional odontodysplasia. (A) Panoramic radiograph of the jaws showing ‘ghost teeth’ in the upper right quadrant; (B) Histological section of decalcified tooth showing malformed tooth with poorly mineralized enamel lacking normal prism structure and atypical dentine with interglobular dentine and increased width of predentine
A wide range of dental anomalies have been reported in EDS. Most commonly these include enamel hypoplasia, large pulpal calcifications or pulp stones, and shortened dilacerated roots (1.9B). The dentine is reported to have abnormal tubular structure. The posterior teeth often have accentuated cusps and fissures. Hypodontia and microdontia and failure of eruption of teeth have also been reported.
Regional Odontodysplasia
This is a nonhereditary localized condition of the jaws with characteristic clinical and radiographic features. The condition involves several adjacent teeth most commonly in a single arch; however, involvement of more than one arch and all teeth has been reported. Deciduous or permanent dentition can be affected and in about half the cases both are involved. There appears to be a slightly higher incidence in females than in males and the maxilla is more commonly involved than the mandible. Association with vascular nevi, hemangioma, epidermal nevus syndrome and hemifacial hypoplasia has been reported in several cases previously.
The most characteristic anomaly is marked hypoplasia of enamel and dentine. Clinically, the teeth are discolored, soft and prone to rapid breakdown. Radiographically, the enamel and dentine are much reduced and the distinction between the two is lost due to poor mineralization, giving appearance of “ghost teeth” (Fig. 1.10A and B). The pulp chambers are enlarged with open apices. Teeth may be missing or fail to erupt. The surrounding soft tissues are often inflamed and there may be periapical inflammation and abscess formation.
Histologically the enamel is thinned and has abnormal prism structure. The dentine is also thinned, with increased width of predentine and presence of interglobular dentine (Fig. 1.10A and B).
The etiology of regional odontodysplasia is unknown. The association with vascular nevi, hemangioma, epidermal nevus syndrome and hemifacial hypoplasia raises the possibility of somatic mutation. Other theories include exposure to teratogenic drugs, vascular or metabolic disturbance, and viral infections.
There is a lack of consensus about the management of regional odontodysplasia. A number of factors need to be considered including the state of the affected teeth, presence of apical infection, whether deciduous or permanent dentition is affected, the need to preserve space for permanent dentition and the compromise in esthetics and function.
DEVELOPMENTAL ABNORMALITIES OF CEMENTUM
Abnormalities of cementum are usually only seen in hypophosphatasia. This is characterized 12by deficiencies of bone mineralization and lack of cellular and acellular cementum associated with a deficiency of the enzyme alkaline phosphatase. The deficiency arises from mutations in the ALPL gene and gives rise to several different clinical forms of the condition of varying severity that corresponds to the severity of the enzyme deficiency. The features are best regarded as a continuum and range from early-onset lethal or severe forms characterized by stillbirth, craniosynostosis, bony deformities hypercalcemia and renal damage to milder, late-onset types characterized by stress fractures and pseudofractures. Premature exfoliation of primary dentition can be seen in isolation (known as odontohypophosphatasia) in the mildest form of the condition or in combination with other features.
DEVELOPMENTAL ABNORMALITIES OF NUMBER OF TEETH
Hyperdontia
Hyperdontia is characterized by increase in one or more teeth in the normal dentition (supernumerary teeth). It can arise in isolation (nonsyndromic) or together with other abnormalities (syndromic). Both primary and secondary dentition may be involved. The prevalence in the Caucasian populations is between 1 and 3 percent but is reported to be higher in Mongoloid races. Presence of multiple supernumerary teeth especially nonsyndromic, is rare. Cases with one or two supernumerary teeth commonly involve the anterior maxilla whilst multiple supernumerary teeth most commonly involve premolar regions in both jaws.
The teeth can be supplemental or rudimentary. Supplemental teeth are of normal size and shape. The most common supplemental teeth are maxillary lateral incisors followed by premolars and molars. Rudimentary teeth are of small size and have an abnormal shape, e.g. conical. The most common supernumerary tooth is mesiodens, a rudimentary conical tooth arising between the permanent maxillary incisors.
Fig. 1.11: Cleidocranial dysplasia. Panoramic radiograph of the jaws showing multiple unerupted supernumerary teeth(Courtesy: Professor K Horner)
Many Mendelian syndromes are associated with supernumerary teeth. The most common of these include cleidocranial dysplasia (Fig. 1.11), familial adenomatous polyposis, orofacial digital syndrome type I, Nance-Horan syndrome, tricho-rhino-phalangeal syndrome, Rothmund–Thomson syndrome and Hallerman–Streiff syndrome.
Supernumerary teeth are often detected as incidental findings on clinical or radiographic examination. However, they can be associated with a number of clinical problems including interference with eruption, displacement, resorption or dilacerations of adjacent teeth, crowding or spacing (diastema), dentigerous cysts and eruption into nasal or antral cavities.
Hypodontia
Hypodontia is characterized by decrease in one or more teeth in the normal dentition. Some authors differentiate this further into complete absence of dentition (anodontia), absence of more than 6 teeth (oligodontia) and absence of less than 6 teeth (hypodontia). The absence of teeth can be in isolation (nonsyndromic) or as part of constellation of features (syndromic).
Hypodontia can affect both primary and permanent dentition. The prevalence in primary dentition is low (about 0.5%) and most commonly involves maxillary incisors lateral incisors followed by mandibular lateral incisors. There is a strong correlation between hypodontia in primary dentition and hypodontia in the permanent dentition.13
The prevalence of hypodontia in the permanent dentition is between 2 and 10 percent. This most commonly (~80% of cases) involves only one or two teeth. Loss of six or more teeth is extremely rare (<0.3% of population). There are racial differences in the pattern of missing teeth; third molars are the most common missing teeth in Caucasians followed by maxillary second premolars and lateral incisors. In contrast, in Mongoloid races, the mandibular incisors are the most common missing teeth. Most studies show a slightly greater incidence of hypodontia in females compared to males.
Hypodontia can occur as result of environmental factors such as local infections, radiotherapy or chemotherapy or other drugs. However, in most cases it is likely to have a genetic etiology. It is often transmitted as an autosomal dominant trait with incomplete penetrance and mutations have been identified in two genes (MSX1 and PAX9) in nonsyndromic hypodontia (1.12A). It is also seen in many Mendelian syndromes including the ectodermal dysplasias (including incontinentia pigmenti) where it is associated with abnormalities of shape of teeth (e.g. conical teeth) (1.12B), in association with predisposition to colorectal cancer, Down syndrome and hemifacial microsomia.
Hypodontia is often associated with other abnormalities such as microdontia (e.g. peg shaped lateral incisors), transposition of permanent teeth, taurodontism and ectopic impacted canines. The principle clinical problems with lack of teeth are lack of function and esthetics coupled with malocclusion.
DEVELOPMENTAL ABNORMALITIES OF ERUPTION OF TEETH
Early Eruption Including Natal Teeth
Early eruption of teeth can occur in isolation or rarely secondary to hyperthyroidism, precocious puberty or as part of a Mendelian syndrome such as Sotos syndrome and pachonychia congenita.
Natal teeth occur in between 1:2000 and 1:3500 live births and more common in females than males. A small percentage (<10%) of these are supernumerary teeth but most are early erupted teeth from the primary dentition. Mandibular central incisors are overwhelmingly the most commonly affected tooth followed by maxillary central incisors. Although natal teeth tend to have a normal shape, they are often smaller, and have dysplastic enamel and dentine with short poorly developed roots with consequent tooth mobility.
The main problems associated with isolated natal teeth are of discomfort to mother when suckling and traumatic sublingual ulceration.
Figs 1.12A and B:
Hypodontia. (A) Panoramic radiograph of the jaws showing a case of nonsyndromic hypodontia with lack of most permanent teeth; (B) Hypohidrotic ectodermal dysplasia with oligodontia and conical tooth
Figs 1.13A to C:
Osteopetrosis. (A) Lateral skull radiograph showing generalized osteosclerosis of the calvarium and skull base, and loss of the frontal sinus; (B) Panoramic radiograph of the jaws showing generalized osteosclerosis with multiple unerupted teeth; (C) Dorsal view radiograph of left hand showing generalized osteosclerosis, and transverse striations and ‘bone-in-bone’ appearance in the phalanges and metacarpus
Delayed or Failure of Eruption of Teeth
This can be syndromic or occur in isolation, can involve single or multiple teeth and affect primary and/or secondary dentition.
Delayed or failure of tooth eruption is seen in many Mendelian syndromes. Some of them can be very loosely grouped into those associated with bony or calcification abnormalities such as osteopetrosis (Fig. 1.13A to C) and cleidocranial dysplasia (see Fig. 1.11), and those associated with growth retardation or atrophy such as hemifacial atrophy, focal dermal hypoplasia and GAPO (growth retardation, alopecia, pseudoanodontia, and optic atrophy). However in other syndromes, e.g. familial adenomatous polyposis (Fig. 1.14), there appears to be no common mechanism of failure of eruption.
Failure of eruption of single teeth is most commonly associated with simple local mechanical obstruction because of dental crowding. Isolated abnormality of eruption without any local or systemic causes and without a family history is known as primary failure eruption. This more commonly affects posterior teeth of both primary and secondary dentition, the involved teeth may fail to erupt completely or may erupt partially and then cease to erupt. This often leads to bony ankylosis of the unerupted or partially erupted tooth.
The main problems associated with failure or delayed eruption, are malocclusion, loss of function, and bony ankylosis of teeth.
Fig 1.14: Familial adenomatous polyposis. Panoramic radiograph of the jaws showing multiple unerupted teeth together with osteomata
DEVELOPMENTAL ABNORMALITIES RESULTING IN EARLY LOSS OF TEETH
These can be broadly divided into three main groups:
- Inherited defects in structure of cementum or periodontium
- Inherited or acquired immune deficiencies of phagocytes
- Stunted or abnormal root development.
There are also forms of early-onset periodontitis where the defect is as yet uncharacterized.
Deficiency of cementum in hypophosphotasia has been described above. Structural abnormality of periodontium resulting in susceptibility to periodontitis and early loss of teeth is seen in some types of Ehlers-Danlos syndromes.15
Immune deficiencies of phagocytes, particularly of neutrophil number and function, are also characterized by gingivitis and destructive early-onset periodontitis. Inherited deficiencies of neutrophil number include congenital neutropenias, cyclic neutropenia and several other syndromes. Acquired neutropenias are associated with hematological malignancies, infections and cytotoxic therapies.
Deficiencies of neutrophil function include defects in chemotaxis (leukocyte adhesion molecule deficiencies), oxidative metabolism (e.g. lack of superoxide dismutase in chronic granulomatous disease, myeloperoxidase deficiency) and protease mediated bactericidal activity (e.g. lysosomal trafficking defects in Chediak-Higashi syndrome, cathepsin C deficiency in Papillon Lefevre syndrome). These conditions usually present in childhood with recurrent infections of skin, lung, liver and bone with pathogenic and normally nonpathogenic bacteria and fungi. Clinical features include fever, recurrent abscesses, lymphadenopathy, hepatosplenomegaly and apthous ulceration.
Stunted or abnormal root development is seen in dentine dysplasia type I, occasionally in dentinogenesis imperfecta and is associated with early loss of teeth.
DEVELOPMENTAL ABNORMALITIES OF TOOTH FORM AND SIZE
Microdontia and Macrodontia
Generalized macrodontia (increase in size of teeth) or microdontia (decrease in size of teeth) is very rare. However, changes in size affecting one or more teeth occur as part of various Mendelian syndromes. For example, conical teeth are observed together with hypodontia in some types of ectodermal dysplasia, a genetically heterogeneous group of disorders characterized by abnormalities of at least two ectodermal derived tissues (commonly skin, hair, nail, eccrine glands and teeth). Similarly, macrodontia involving canine and molar teeth is seen in otodental syndrome together with sensorineural deafness and coloboma. Isolated microdontia is observed in about 1 percent of population and commonly affects 3rd molars and maxillary lateral incisors.
Dens Invaginatus
Dens invaginatus or dens-in-dente is developmental malformation thought to arise by infolding of the dental papilla and characterized by enamel-lined cavity extending to a variable depth into the body of the tooth (Fig. 1.15A and B).
Figs 1.15A and B: (Courtesy forFigure 15B: Dr K Hunter)
Dens-in-dente. (A) Periapical radiograph showing tooth inside a tooth appearance; (B) Longitudinal histological ground section showing tooth dilated by an enamel lined cavity extending into the pulp space
16In its least severe form, it forms a small pit in the enamel or an enamel-lined sac that extends into the dentine and is confined with the crown. In the more severe form, the inversion extends into the pulp and may, or may not communicate with pulp. In the most severe type, the inversion extends through the root laterally or apically and forms a second foramen in the periodontium or at the apex respectively.
The reported prevalence of the dens invaginatus in full mouth surveys is between 0.5 and 10 percent. The anomaly is usually seen in permanent teeth although occasionally it has been reported in deciduous and even supernumerary teeth. The most commonly affected teeth are maxillary lateral incisors followed by maxillary central incisors and canines.
Clinically the first presentation is often because of pulpitis or periapical infection due to communication between the pulp and invagination or secondary to caries in the invagination. Depending on the severity of the invagination, the tooth may appear to have normal morphology or may be markedly expanded to accommodate the invagination. Similarly, changes on radiographic examination may be quite subtle or marked. Endodontic treatment is normally required but may be difficult because of quite complex root morphology.
Dens Evaginatus and Enamel Pearls
Dens evaginatus is a developmental abnormality characterized by an accessory cusp consisting of enamel and dentine and in about half the cases, extension of the dental pulp. This abnormality is more common in people of Asian, North American Eskimo and Native American populations with reported incidence between 0.5 and 15 percent.
Dens evaginatus most commonly occurs on the occlusal surface of molars and the lingual surface of anterior teeth. Where the cusp is particularly prominent in anterior teeth it is referred to as a talon cusp (Fig. 1.16). The clinical significance of dens evaginatus is that because of its site, it is in occlusion and therefore suffers wear or fracture due to occlusal pressure resulting in pulp exposure.
Fig 1.17: Enamel pearl. Solitary small hard tissue nodule consisting of enamel at bifurcation of a maxillary second molar
Enamel pearls are small hard tissue nodules consisting of enamel usually with a core of dentine rarely pulp, and are found on roots of deciduous and permanent teeth (Fig. 1.17). They are usually solitary and commonly found at bifurcation of molars particularly maxillary, second and third permanent molars. Prevalence of between 1 and 10 percent has been reported. Clinically they are of little significance although 17a few studies suggest that they may act as plaque retention factors and predispose to local gingivitis or periodontitis.
Taurodontism
Taurodontism is characterized by increase in size of pulp chamber with apical displacement of the pulp chamber floor and loss of cervical constriction (Fig. 1.18). The anomaly most commonly occurs in isolation but is also seen in many chromosomal and Mendelian syndromes including Down syndrome, Klinefelter's syndrome and tricho-osseous-dental syndrome.
Fig 1.18: Taurodontism. Periapical radiograph showing molar tooth with increase in size of pulp chamber, apical displacement of the pulp chamber floor and loss of cervical constriction
The reported prevalence of the condition varies markedly (5.4–65%) probably due to differences in the diagnostic criteria, and the teeth and the populations assessed.
As the crown morphology is normal, taurodontism is most commonly detected as an incidental finding on radiographs taken for routine dental care. Taurodontism is of little clinical significance other than exclusion of any syndromes and possible difficulties in endodontic treatment of affected teeth.
Gemination
Gemination is defined as an attempt by a single tooth bud to form two teeth resulting in a bifid crown with a single root (Fig. 1.19A and B). There is no variation in the number of teeth if the bifid tooth is counted as a single tooth. Prevalence is reported to be less than 1 percent and few bilateral cases have been reported. As with fusion, gemination is largely in the anterior dentition and gemination in the primary dentition is followed in about half the cases with gemination of the succedaneous permanent teeth.
Fusion
Dental fusion is defined as a union of two adjacent teeth involving dentine and/or enamel.
Figs 1.19A and B: Gemination. (A) Bifid crown upper lateral incisor; (B) Periapical radiograph showing bifid crown with partial single root in upper lateral incisor
The fusion is usually between teeth in the normal dentition although occasionally involves a supernumerary tooth. Depending on the timing of the fusion can be total or partial, the latter just involving the roots. The primary dentition is more commonly affected and the prevalence is reported to be 0.5 to 2.5 percent. It is seen almost exclusively in the anterior dentition and fusion in the primary dentition is followed in about half the cases with fusion of the succedaneous permanent teeth.
Dental fusion usually occurs in isolation but is also observed in one Mendelian syndrome, oculocardiofacial dental syndrome, an X-linked male-lethal, recessive condition with widespread abnormalities (Fig. 1.20).
Concresence
Concresence is fusion of the roots of teeth by hypercementosis. This is a rare condition usually affecting maxillary second and third molars. Cause is unknown but it is thought to be due to hypercementosis, secondary to chronic apical inflammation or associated with roots of impacted third molars that are positioned in close proximity to the roots of the second molars. There is no clinical significance other than difficulty in extraction of the teeth involved.
BASIC PRINCIPLES AND MANAGEMENT OF PATIENT WITH DEVELOPMENTAL ANOMALIES OF TEETH
Management of a patient presenting for the first time with a developmental abnormality of the teeth will naturally depend on the abnormality. However, we can define some basic principles that are important in management of such patients. Detailed exposition of the treatment of all developmental anomalies of teeth is beyond the scope or remit of this chapter and only a very general guidance is provided.
It is important at the outset to appreciate that the management of patients with these conditions requires multidisciplinary expertise and input. A good clinician will recognize his, or her own limitations and seek help from other relevant specialists.
Commonly, the first presentation of any significant developmental abnormality of teeth is during childhood so the guidance below is provided in this context. Additionally, often the phenotype is distinctive, and will indicate the diagnosis and define the relevant course of management. The clinical pathway through which the patients present will depend on the nature and severity of the condition. Patients with more severe phenotypes (i.e. those with more marked systemic features) are likely to present with a possible or definitive diagnosis by referral from specialist medical practitioners. In contrast, those with predominantly dental changes or with latent or subtle (but not necessarily insignificant) system manifestations may present first to the dental practitioner. Thus it is important that the dental practitioner is able to not only recognize the dental phenotype but also appreciate the significance of these changes in the wider context and the implications they may have on the patient's general well-being. A good example of this is the dento-osseous changes seen in familial adenomatous polyposis, an autosomal dominant condition associated with colorectal polyposis that almost inevitably leads to colorectal carcinoma. The dento-osseous changes may be detected well in advance of development of any colorectal signs and symptoms and provide an opportunity for prophylactic and potentially lifesaving intervention.
Comprehensive history is vital to ascertain whether the condition is acquired or genetic, isolated or part of a syndrome and sporadic or familial. In determining whether the condition is acquired or genetic, unless the phenotype 19is so distinctive as to suggest the diagnosis, it is important to establish history of relevant exposure to environmental agents (infections or drugs for example) during the developmental phase of the teeth affected. For primary dentition, this will of course include history of exposure of the mother during pregnancy.
A full medical history is essential in determining whether the condition is part of a syndrome. It should include eliciting history of specific features associated with the suspected condition even if medical treatment has not been sought for this, as the parent may not recognize this as significant or associate them with oral or dental changes.
A detailed family history should be elicited tracing back if possible at least two generations and a pedigree constructed indicating age and status if known of all members. This will help identify the mode of inheritance and also members of the family who may be at risk of having the condition or being carriers of the condition.
Nature of examination of patient will depend on the setting and expertise of the dental practitioner. At the very least, any obvious dysmorphic features or other general abnormalities should be noted. Examination of teeth should include accurate description of abnormality and teeth affected. Special tests will depend on the nature of the abnormality, age of the patient and nature of the condition. In young children, intrusive tests should only be pursued if there is possibility of therapeutic benefit or need for surveillance. Otherwise consideration should be given to postponing the tests until child is old enough to understand and able to consent.
For patients with a genetic condition, referral to a clinical geneticist is essential so that patients and their families can receive genetic counseling and information about recurrence risks. This is particularly important for conditions associated with potentially significant systemic features. Definitive diagnostic information for such conditions should be given to the patients together with, or by a clinical geneticist.
Treatment will clearly depend on the nature of the abnormality and may involve one or more dental specialists. Prevention of caries and/or periodontal disease is likely to be essential in many of the conditions.
ACQUIRED ABNORMALITIES OF TEETH
Attrition
Physiological attrition is an irreversible loss of dental hard tissue by wearing away of the tooth surface by tooth-to-tooth contact. Pathological attrition resulting in excessive loss of tooth surface is seen in association with parafunctional habits such as bruxism. The prevalence of severe attrition (involving dentine) in adults increases from about 3 percent at age of 20 years to 17 percent at age of 70 years. In children, a wide variation in prevalence has been reported for severe wear of the deciduous dentition ranging from 0 to 82 percent.
Clinically attrition is seen as matching wear facets on opposing teeth (Fig. 1.21). Commonly these are on the occlusal surface but can affect buccal and lingual surfaces with certain types of malocclusions. Excessive loss may result in a loss of occlusal face height (or vertical dimension of occlusion), thermal sensitivity due to exposure of dentine and poor esthetics.
Treatment for attrition will depend on the extent of tooth surface loss, etiology, symptoms, whether loss is progressive or stable, and the level of compromise of esthetics. Management of etiological factors such as correction of malocclusion and treatment of parafunctional habits should precede any restorative procedures.
Fig. 1.21: Dental attrition. Excessive loss of tooth surface seen as wear facets on the occlusal and incisal surface of teeth(Courtesy: Dr S Al-Salehi)
20Sensitive dentine may be treated by topical application of varnishes and use of desensitizing toothpastes.
Abrasion
Abrasion is an irreversible loss of dental hard tissue by mechanical wear of tooth substance by factors other than tooth-to-tooth contact such as food, toothpastes or toothbrushing. The prevalence of tooth loss solely due to abrasion is difficult to determine from the reported literature. It is now widely recognized that abrasion and erosion probably act in concert to cause tooth loss. Clinical and laboratory evidence suggests that abrasion alone is unlikely to cause significant tooth wear. The prevalence of noncarious cervical wear classically attributed to toothbrush abrasion is reported to be between 5 and 85 percent. This wide discrepancy is due to different parameters used to assess the loss. Loss of tooth surface limited to enamel is relatively common with prevalence ranging from 13 to 100 percent. However, prevalence of loss involving dentine is likely to be much lower at ⩽5 percent.
Clinical presentation of lesions resulting from abrasion (together with erosion) depends on the etiological factors. As mentioned above, noncarious cervical lesions are associated with toothbrush abrasion. They are almost always on the outer or vestibular surface of teeth, and affect maxillary anterior and premolar teeth predominantly (Fig. 1.22). The lesions can have variable depth and either smooth or sharp profiles. They are usually associated with dentinal sensitivity.
Fig. 1.22: Dental abrasion. Partly restored abrasion cavities on the cervical margins of the buccal surfaces of teeth(Courtesy: Dr S Al-Salehi)
Treatment involves correction of etiological factors, application of dentine bonding agents to reduce sensitivity and restorative treatment depending on the depth of the lesions.
Erosion
Erosion is irreversible loss of dental hard tissue by action of chemicals but not involving dental plaque acids or caries. As mentioned above, erosion co-exists with abrasion and attrition, and contribution of any individual component may be difficult to determine. Erosion is seen in both children and adults. Primary dentition is thought to be more susceptible to erosion than permanent dentition because of the thinner layer of enamel in the former. The reported prevalence figures vary greatly; the incidence in younger children is thought to be approximately ⩽10 percent rising with age to approximately 50 percent.
There are a number of proposed intrinsic and extrinsic sources of acids. The former include gastroesophageal reflux and persistent vomiting. Gastroesophageal reflux disease or GORD is a fairly common condition reported in up to 20 percent of the population in the developed countries. It is widely accepted amongst the dental community that GORD is associated with dental erosion and an increased prevalence of dental erosion has been reported previously in patients with GORD. However a recent systemic review suggested that there is no evidence of a strong link between GORD and dental erosion.
Self-induced or spontaneous persistent vomiting can also result in erosion of tooth surface. Recurrent spontaneous vomiting is relatively uncommon. In children and more rarely in adults, cyclic vomiting (known as cyclic vomiting syndrome) is associated with migraine, abnormal gastrointestinal motility or several other disorders. Self-induced vomiting is more common and is usually observed in female teenagers or young adults as part of anorexia and bulimia nervosa.
There are several extrinsic factors in the etiology of dental erosion. Consumption of acidic drinks and to a lesser extent, acidic foods 21is emerging to be a significant factor. Acidic medications or illicit drugs such as ecstasy have also been reported to be associated with dental erosion. There is likely to be a greater susceptibility to dental erosion with long term drug therapy, with xerostomia-inducing drugs and consequent loss in the buffering effect of the saliva although there is no strong evidence to support this. A systemic review of occupational exposure to acids concluded that evidence of association with dental erosion is limited to battery and galvanizing workers (with limited data to support association with exposure in other areas such as chemical and pharmaceutical industries).
Clinically, dental erosion shows variable appearances. These include a smooth shiny rounded surface, surface depressions often with irregular ridges, cusp or incisal tip thinning and fracture, exposure of dentine with change of tooth color from white to yellow and at later stages thermal sensitivity. Commonly maxillary anterior teeth are involved; the most common sites on the teeth are palatal, incisal and occlusal surfaces (Fig. 1.23A to C).
Cornerstone of management is identification and removal of the etiological factor(s). Where a systemic cause is suspected, liaison with an appropriate specialist is important. Dietary monitoring (using diet diaries) and counseling, oral hygiene instruction, remineralization of the tooth surface with fluoride toothpastes, mouthwashes and varnishes, and application of dentine bonding agents to reduce sensitivity all have a role in treatment. In the more severe cases, restorative treatment may be necessary (O'Sullivan and Milosevic, 2008).
Abfraction
Abfraction is defined as the pathological loss of tooth substance caused by biomechanical loading forces that result in flexure and failure of enamel and dentin at a location away from loading. This is thought by some to be the primary etiological factor for wedge shaped cervical lesions traditionally attributed to abrasion and erosion. It is postulated that tensile stress on teeth during mastication, in malocclusion and parafunctional habits such as bruxism can concentrate at the cemento-enamel junction and lead to tooth breakdown at this site. In addition, the tensile stresses can pull apart the enamel prisms making the surface more vulnerable to acid erosion. The evidence for this is largely based on engineering models. There is no convincing evidence that abfraction acts as a primary factor in inducing cervical lesions and it is widely accepted that these lesions arise through a multifactorial etiology with erosion and abrasion playing a significant role.
INTERNAL AND EXTERNAL ROOT RESORPTION
Pathological root resorption is defined as loss of tooth surface on the inside or outside of the root (internal or external root resorption respectively) by clastic activity.
Root resorption is thought to consist of two phases, injury and stimulation. The first phase is injury to the nonmineralized tissues such as predentine and precementum on the tooth surface with exposure of mineralized tissue to clastic cells of monocyte-macrophage series. This leads to colonization of the tooth surface by clastic cells and limited resorption of the hard tissues.
Figs 1.23A to C: Dental erosion affecting occlusal, palatal and incisal surfaces(Courtesy: Dr S Al-Salehi)
22However, this will only continue in presence of stimulation of clastic activity by, e.g. inflammation or pressure.
Several different types of processes are involved in root resorption:
- Inflammatory resorption associated with marked inflammation
- Replacement resorption associated with mild inflammation and characterized by attempted repair with metaplastic hard tissues
- Surface resorption associated with sustained pressure
- Ankylosing resorption associated with severe trauma resulting in exposure of a large area of mineralized dentine to osteoclasts with consequent root resorption and replacement by bone.
Internal Root Resorption
Internal root resorption can be apical or intraradicular. The former is the more common and seen together with apical external root resorption in up to 75 percent of teeth with periapical infection and inflammation. Intraradicular root resorption is relatively rare in permanent dentition and may be associated with pulpitis, trauma or autotransplantation. This type of resorption is characterized by replacement with metaplastic osteocementum.
Early internal resorption often has no specific features and may be detected as an incidental finding on radiographs. The presenting signs and symptoms may be those associated with the etiological factors, i.e. pulpitis, periapical inflammation or trauma. In more advanced internal root resorption, there may be pink discoloration of the crown associated with coronal intraradicular root resorption, sinus tracts associated with root perforation, or mobility of the crown associated with root fracture.
External Root Resorption
Several specific types of external root resorption are seen.
Cervical external root resorption is thought to be associated with inflammation in the periodontium. This may be a consequence of bacterial irritation or mechanical trauma. It has also been reported to occur more frequently in endodontically treated teeth where a bleaching agent was used in preparation of the root canal. It is thought that the bleaching agents leach through the dentinal tubules into the periodontium causing local injury. In most cases with early cervical lesions, there are no symptoms. In teeth with more advanced lesions with larger resorption cavities, there may be thermal sensitivity or pink discoloration of the crown at the cervical margin as the enamel is undermined by granulation tissue. Affected teeth have vital pulp and exposure of the pulp and symptoms of pulpitis may only occur at a late stage. Radiographically, cervical external root resorption is detected as an irregular cervical radiolucency through which the mineralized intact outline of the pulp chamber and root canals is visible (Fig. 1.24A and B).
Figs 1.24A and B: External root resorption. (A) Extracted upper central incisor with external root resorption; (B) Periapical radiograph showing an upper central incisor with external root resorption
23Management of cervical external resorption involves exposure of the erosion cavity, debridement, treatment with calcium hydroxide and placement of restoration. Endodontic treatment is only necessary where there is pulpal involvement.
Inflammatory external resorption along the length of the root and at the apex of the tooth can also occur in association with pulpitis and apical periodontitis. Radiographically, this is seen as irregular erosions of root surface. Management is by endodontic treatment.
Pressure-related symmetrical external root resorption in the apical third of teeth is sometimes seen as a consequence of orthodontic treatment. There may be significant shortening of the roots but the teeth are vital and symptomless. Similarly, resorption due to pressure from tumors, cysts or impacted teeth results in localized resorption in an area of pressure but the affected teeth are vital and symptomless.
Ankylosing-type of external root resorption occurs as a consequence of severe trauma such as intrusive luxation or reimplantation after lengthy delay following avulsion. The affected tooth is symptomless and may show reduced physiological mobility. Radiographically, the resorption cavities on the root surface are filled in by bone and there is a loss of periodontal ligament space.
TOOTH DISCOLORATION AND STAINING
Changes in the appearance of the color of the teeth may be due to intrinsic tooth discoloration, external staining or internalized discoloration.
Intrinsic Discoloration
This can arise from:
- Developmental structural abnormalities of teeth
- Incorporation of color imparting substances in the hard tissues during development.
Inherited and acquired developmental structural abnormalities of enamel and dentine that alter the appearance of teeth have been discussed above. These include amelogenesis imperfecta, environmental enamel hypoplasia including fluorosis, dentinogenesis imperfecta and dentine dysplasia.
Fig 1.25: Intrinsic discoloration of teeth. Tetracycline staining of teeth imparting yellow discoloration to newly erupted teeth that changes to gray-brown discoloration on exposure to sunlight
Color imparting substances derived from intrinsic and extrinsic sources may be incorporated into the developing dentition. Extrinsic substances include tetracycline that complexes with calcium ions on the surface of hydroxyl apatite crystals. The discoloration will depend on the type of tetracycline, dose and the period of use. Most commonly the staining will appear as a discrete bright yellow to gray or brown band at eruption but will change over time on exposure to sun (Fig. 1.25).
Intrinsic sources of discoloration include metabolic products. In alkaptonuria, an autosomal recessive condition characterized by a deficiency of enzyme involved in tyrosine breakdown results in accumulation of homogentisic acid which imparts a brown discoloration to teeth. In congenital erythropoietic porphyria, an autosomal recessive condition in which there is deficiency of enzyme necessary for heme production, there is build of porphyrin precursors that impart red-brown discoloration to teeth and red fluorescence under UV light. Similarly conditions in which there is extensive hemolysis or hyperbilirubinemia during the period of dental development can lead to deposition of biliverdin in teeth and yellow discoloration.
Extrinsic Staining
This can arise from either from the intrinsic color of substances incorporated into the dental 24pellicle or from color generated by reaction of substances at the tooth surface.
There are numerous sources of chromogens in the mouth including foods, drinks (tea, coffee, wine), mouthrinses (chlorehexidine in particular) and medications such as iron supplements. Occupational exposure to metal salts such as iron and copper can impart distinctive black or green discoloration respectively.
Internalized Staining
Unlike intrinsic discoloration, this arises through internalization of chromogens into the tooth substance after development of the tooth is complete. Factors that increase the porosity of the surface enamel or expose dentine such as acquired or inherited developmental defects, or dental caries can predispose to internalized staining. In addition to chromogens in foodstuffs, drinks, etc. tin from dental amalgam can also be internalized and discolor teeth with longstanding restorations.
SELF-ASSESSMENT QUESTIONS
- Define amelogenesis imperfecta and explain how the clinical presentation reflects the underlying genetic basis.
- Define environmental enamel hypoplasia and describe three common examples.
- Define dentinogenesis imperfect and describe the three most common types.
- Describe two conditions which result in abnormalities of both enamel and dentine.
- Classify, and describe with examples, abnormalities of tooth number.
- Discuss the causes of delayed or failure of eruption of teeth.
- Describe the causes of early loss of teeth.
- Describe five developmental abnormalities of tooth size and form.
- Describe the four forms of noncarious tooth surface loss.
- Discuss the causes of intrinsic staining.
SUGGESTED READING
- Brook AH. Multilevel complex interactions between genetic, epigenetic and environmental factors in the aetiology of anomalies of dental development. Archives of Oral Biology. 2009;54(Suppl 1):S3-S17.
- I Bailleul-Forestier, Molla M et al. The genetic basis of inherited anomalies of the teeth: Part 1: Clinical and molecular aspects of non-syndromic dental disorders. European Journal of Medical Genetics. 2008;51(4):273–91.
- I Bailleul-Forestier, Berdal A et al. The genetic basis of inherited anomalies of the teeth: Part 2: Syndromes with significant dental involvement. European Journal of Medical Genetics. 2008;51(5):383–408.
- Thesleff I. The genetic basis of tooth development and dental defects. American Journal of Medical Genetics. 2006; Part A 140A(23): 2530–5.