SKELETON
Parts of Bone
Bone is a calcified connective tissue consisting of cells (osteocytes) embedded in a matrix of ground substance and collagen fibers.
- It has a superficial thin layer of compact bone around a central mass of spongy bone, and contain internal soft tissue, the marrow, where blood cells are formed.
- It serve as a reservoir for calcium and phosphorus and act as biomechanical levers on which muscles act to produce the movements permitted by joints.
Long bones have a shaft (diaphysis) and two ends (epiphyses). The metaphysis is a part of the diaphysis adjacent to the epiphyses.
- Diaphysis
- Forms the shaft (central region) and is composed of a thick tube of compact bone that encloses the marrow cavity.
- Metaphysis
- Is a part of the diaphysis, the growth zone between the diaphysis and epiphysis during bone development.
- Epiphyses
- Are expanded articular ends, separated from the shaft by the epiphyseal plate during bone growth and composed of a spongy bone surrounded by a thin layer of compact bone.
Bones in the Body
- Bony skeleton consists of 206 bones and is divided into two parts: the axial skeleton and the appendicular skeleton.
- Axial skeleton is the central core unit, consisting of the skull, vertebrae, ribs, and sternum.
- Appendicular skeleton comprises the bones of the extremities.
Sesamoid Bones
Sesamoid bones develop in certain tendons and reduce friction on the tendon, thus protecting it from excessive wear.
- They are commonly found where tendons cross the ends of long bones in the limbs.
- Sites of sesamoid bones:
- In the ear: The lenticular process of incus is a sesamoid bone and therefore is considered the fourth ossicle of middle ear.
- In the hand: Two sesamoid bones in the distal portions of the first metacarpal bone (within the tendons of adductor pollicis and flexor pollicis brevis).
- In the wrist: The pisiform of the wrist is a sesamoid bone (within the tendon of flexor carpi ulnaris), develops at age 9–12.
- In the knee: The patella (within the quadriceps tendon)
- Fabella in the lateral head of gastrocnemius behind the knee joint.
- Sesamoid bone in the tendon of peroneus longus where it binds around the cuboid bone.
- In the foot: Two sesamoid bones in the distal portions of the first metatarsal bone (within the tendons of flexor hallucis brevis.
Pneumatic Bones
Note: Pneumatic bones are the irregular bones which contain air-filled cavities within them.
- They are generally produced during development by excavation of bone by pneumatic diverticula (air sacs) from an air-filled space such as the nasal cavity.
- E.g., maxilla, frontal, sphenoid, and ethmoid bones and a part of the mastoid process of the temporal bone.
Note: At birth the mastoid is not pneumatized, but becomes aerated over the first year of life.
Ossification
- Ossification is the process of laying down new bone material by cells called osteoblasts. It is of two types:
- Membranous ossification is the direct laying down of bone into the mesenchyme (embryonic connective tissue).
- Endochondral ossification involves osteogenesis in a precursor model of cartilage.
- Membrane (dermal) bones ossify in membrane (intramembranous ossification), and are thus derived from mesenchymal condensations. The flat bones of the skull and face, the mandible, and the clavicle develop by intramembranous ossification.
- Cartilaginous bones ossify in cartilage (endochondral ossification), and are thus derived from preformed cartilaginous models. The bones of the extremities (limbs) and those parts of the axial skeleton that bear weight (vertebral column and thoracic cage) develop by endochondral ossification.
- Membrano-cartilaginous bones are initially formed in membrane but later partly in cartilage. Examples: clavicle, mandible, occipital, temporal, sphenoid.
- Cartilaginous ossification involves primary and secondary centres of ossification:
- Primary center of ossification
- In long bones, bone tissue first appears in the diaphysis (middle of shaft).
- Primary centres starts appearing at week 6 of intrauterine life.
- Chondrocytes multiply and form trabeculae and cartilage is progressively eroded and replaced by bone, extending towards the epiphysis.
- A perichondrium layer surrounding the cartilage forms the periosteum, which generates osteogenic cells that make a collar to encircles the exterior of the bone and remodels the medullary cavity on the inside.
- The nutrient artery enters via the nutrient foramen from a small opening in the diaphysis.
- It invades the primary centre of ossification, bringing osteogenic cells (osteoblasts on the outside, osteoclasts on the inside.)
- The canal of the nutrient foramen is directed away from more active end of bone when one end grows more than the other.
- When bone grows at same rate at both ends, the nutrient artery is perpendicular to the bone.
- Secondary center of ossification
- The secondary centres generally appear at the ends (epiphysis) of long bones.
- Secondary ossification mostly occurs after birth except for secondary centers around knee joint (distal femur and proximal tibia), which appear during last weeks of fetal life (or immediately after birth).
- The epiphyseal arteries and osteogenic cells invade the epiphysis, depositing osteoblasts and osteoclasts which erode the cartilage and build bone. This occurs at both ends of long bones but only one end of digits and ribs.
Ossification centers which appear prenatally (ossified at birth) are: diaphysis of long bones, skull bones, vertebral column, ribs and sternum, few foot bones (talus, calcaneum, cuboid).
Primary center of all carpal and tarsal bones (except talus, calcaneum and cuboid) appear after birth.3
Figs. 2A and B: Growth of bone—lengthwise: (A) Four zones of epiphyseal cartilage, (B) Conversion of calcified cartilage into bone
Time period | Bones affected |
|---|---|
Second month of fetal development | Ossification in long bones beginning |
Fourth month | Most primary ossification centers have appeared in the diaphyses of bone. |
Birth to 5 years | Secondary ossification centers appear in the epiphyses |
5 years to 12 years in females, 5 to 14 years in males | Ossification is spreading rapidly from the ossification centers and various bones are becoming ossified |
17 to 20 years | Bone of upper limbs and scapulae becoming completely ossified |
18 to 23 years | Bone of the lower limbs and os coxae become completely ossified |
23 to 25 years | Bone of the sternum, clavicles, and vertebrae become completely ossified |
By 25 years | Nearly all bones are completely ossified |
Growing End
- The growing ends of bones in upper limb are upper end of humerus and lower ends of radius and ulna.
- In lower limb, the lower end of femur and upper end of tibia are the growing ends.
- The nutrient foramen is directed away from the growing end of the bone; their directions are indicated by a memory aid: ‘Towards the elbow I go, from the knee I flee’.
Blood Supply
Nutrient artery enters the diaphysis (shaft) through the nutrient foramen, runs obliquely through the cortex, and divides into ascending and descending branches in the medullary cavity.
- Each branch divides into a number of small parallel channels which terminate in the adult metaphysis by anastomosing with the epiphysial, metaphysial and periosteal arteries.
- It supplies medullary cavity, inner 2/3 of cortex and metaphysis.
- The nutrient foramen is directed away from the growing end of the bone. Memory aid: Towards the elbow I go, from the knee I flee.
ASSESSMENT QUESTIONS
- Bones ossified at birth: (PGIC 2015)a. Lower end of femurb. Calcaneumc. Upper end of tibiad. Upper end of humeruse. Lower end of humerus
- Endochondral ossification is/are seen in: (PGIC 2015)a. Long bonesb. Flat bones of skullc. Clavicled. Mandiblee. Nasal bones
- Nutrient artery runs: (NEET Pattern 2012)a. Towards metaphysisb. Away from metaphysisc. Away from epiphysisd. None
ANSWERS AND EXPLANATIONS
- a. Lower end of femur; b. Calcaneum; c. Upper end of tibia
- Secondary centers around knee joint (distal femur and proximal tibia) appear during last weeks of intrauterine life (or immediately after birth).
- Primary center of all tarsal bones (except talus, calcaneum and cuboid Appear after birth.
- a. Long bones
- Long bones develop by endochondral ossification, whereas bones of skull; facial skeleton; mandible; clavicle bone develop by membranous ossification.
- a. Towards metaphysis
- Nutrient artery enters the shaft (diaphysis) of the bone, divides into ascending and descending branches, which run towards and terminate in the adult metaphysis by anastomosing with the epiphyseal, metaphyseal and periosteal arteries.
Epiphysis
There are four types of epiphysis:
- Pressure epiphysis are the parts of bone involved in weight transmission (and are intracapsular) for e.g. head of humerus and femur and condyles of humerus, femur, tibia etc.
Figs. 6A to D: Types of epiphyses: (A) Pressure and traction epiphyses. (B) and (D) Atavistic epiphyses. (C) Aberrant epiphysis
- Traction epiphysis are present at the ends of bones and develop due to traction by the attached muscles (and are therefore extracapsular), e.g. greater (and lesser) tubercles in humerus and greater (and lesser) trochanter in femur.
- These epiphyses ossify later than pressure epiphyses.
- Examples of traction epiphyses are tubercles of the humerus (greater tubercle and lesser tubercle), and trochanters of the femur (greater and lesser). Mastoid process is also a traction epiphysis.
- Atavistic epiphysis: These types of fused bones are called atavistic, e.g. the coracoid process of the scapula, which has been fused in humans with the main bone, but is separate in lower animals.
- Aberrant epiphysis: These epiphyses are deviations from the normal anatomy and are not always present. For example, the epiphysis at the head of the first metacarpal bone, posterior tubercle of talus (as trigonum).
ASSESSMENT QUESTIONS
- Which of the following is a traction epiphysis? (NEET Pattern 2012)a. Tibial condylesb. Trochanter of femurc. Coracoid process of scapulad. Head of femur
- Traction epiphysis is/are: (PGIC)a. Head of humerusb. Lesser tuberclec. Deltoid tuberosityd. Coracoid processe. Greater trochanter
-
a. Coracoid processb. Greater tubercle of humerusc. Base of 1st metacarpald. Base of 2nd metacarpal
- Mastoid process is which type of epiphysis? (NEET Pattern 2015)a. Pressureb. Aberrantc. Atavisticd. Traction
ANSWERS AND EXPLANATIONS
- b. Trochanter of femur
- Trochanter of femur is an example of traction epiphysis and is extracapsular.
- Tibial condyles and head of femur are under the pressure epiphysis category and are intracapsular.
- Coracoid process of scapula is an example of atavistic epiphysis.
- b. Lesser tubercle; e Greater trochanter.
- Traction epiphysis are present at the ends of bones and develop due to traction by the attached muscles (and are therefore extracapsular), e.g. Greater (and lesser) tubercles in humerus and greater (and lesser) trochanter in femur.
- Pressure epiphysis are involved in weight transmission (and are intracapsular) for e.g. head of humerus and femur and condyles of humerus, femur, tibia etc.
- Coracoid process in scapula is an example of atavistic epiphysis.
- Deltoid tuberosity is not an epiphysis (it is present on the shaft/diaphysis).
- d. Base of 2nd metacarpal
- Aberrant epiphyses are deviations from the normal anatomy and are not always present. For example, the epiphysis at the head of the first metacarpal bone and at the bases of other metacarpals.
- d. Traction
- Traction epiphysis are present at the ends of bones and develop due to traction by the attached muscles (and are therefore extracapsular).
- Mastoid process is produced due to the traction by the sternocleidomastoid muscle.
Miscellaneous
ASSESSMENT QUESTIONS
- All of the following statements are true for metaphysis of bone EXCEPT: (AIPG 2003)a. It is the strongest part of boneb. It is the most vascular part of bonec. Growth activity is maximized hered. It is the region favoring hematogenous spread of infection
- All of the following statements are true for metaphysis of bone EXCEPT: (AIPG 2003)a. It is the epiphyseal end of diaphysisb. Growth activity is negligible herec. It is highly vasculard. Common site of osteomyelitis in children
- TRUE statement is: (AIPG 2000)a. Osteoblasts give rise to osteocytesb. Growth of bone occurs at diaphysisc. Epiphysis is present between metaphysis and diaphysisd. Interphalangeal joint is a saddle joint
- Pisiform is which type of bone? (NEET Pattern 2015)a. Pneumatic boneb. Sesamoid bonec. Accessory boned. Long bone
- All of the following are pneumatic bones EXCEPT: (AIPG 2011)a. Frontalb. Ethmoidc. Mandibled. Maxilla
- Bone which is pneumatic: (PGIC May 2015)a. Maxillaryb. Parietalc. Temporald. Frontale. Ethmoidal
ANSWERS AND EXPLANATIONS
- a. It is the strongest part of bone
- The strongest part of bone is diaphysis (not metaphysis).
- During growth of bone maximum activity occurs at growth plate (physis) and metaphysis.
- Metaphysis is the most vascular part of bone and most prone for lodging of the infectious agent in hematogenous infection.
- b. Growth activity is negligible here
- Metaphysis is the epiphyseal end of the diaphysis.
- Growth activity is maximum at the growth plate (physis) and metaphysis.
- Metaphysis is richly supplied with arteries forming hairpin bends, hence becomes a common site of osteomyelitis in children, as infectious agent are easily trapped in sluggish blood flow in hairpin bends.
- a. Osteoblasts give rise to osteocytes
- Osteoblasts that get trapped in Haversian lamellae become osteocyte and assume the function of bone maintenance. They are no longer involved in bone formation.
- Growth activity is maximum at the growth plate (physis) and metaphysis.
- Metaphysis is present between diaphysis and epiphysis.
- Interphalangeal joint is a hinge variety of synovial joint.
-
- Sesamoid bones develop in certain tendons and reduce friction on the tendon, thus protecting it from excessive wear.
- They are commonly found where tendons cross the ends of long bones in the limbs.
- c. Mandible
- Pneumatic bones have air spaces within them.
- It is generally produced during development by excavation of bone by pneumatic diverticula (air sacs) from an air-filled space such as the nasal cavity.
- a. Maxillary; c. Temporal; d. Frontal; e. Ethmoidal
- Pneumatic bones have air spaces within them and are present around the nasal cavity.
- Parietal bone is not a pneumatic bone.
Joints
Union between bones can be in one of three types: by fibrous tissue; by cartilage; or by synovial joints.
Classification
Synarthrosis (immovable) | Fibrous joints |
Amphiarthrosis (slight mobile) | Cartilaginous joint |
Diarthrosis (freely mobile) | Synovial joints |
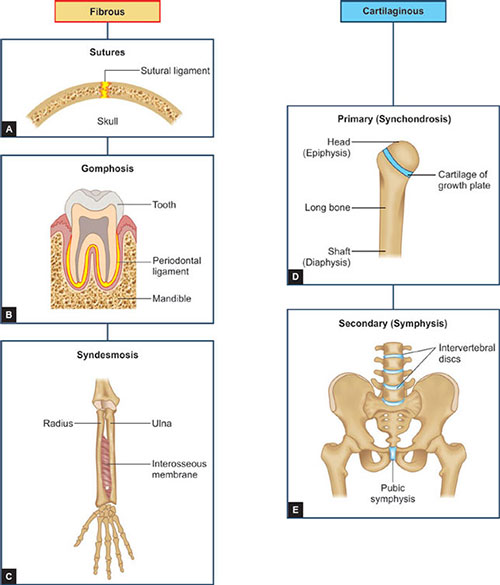
Fibrous joints occur where bones are separated only by connective tissue and movement between them is negligible. Examples of fibrous joints are the sutures that unite the bones of the vault of the skull and the syndesmosis between the lower ends of the tibia and fibula.
Types of fibrous joint | Examples |
Suture | Spheno-vomerine joint (schindylesis) |
Gomphosis | Tooth and socket joints |
Syndesmosis | Middle radioulnar joint Inferior radioulnar joint |
Cartilaginous joints are of two varieties, primary and secondary.
- Primary Cartilaginous Joints (synchondroses) are united by hyaline cartilage and permit no movement but growth in the length.
- A primary cartilaginous joint (synchondrosis) is one where bone and hyaline cartilage meet. Thus all epiphyses are primary cartilaginous joints, as are the junctions of ribs with their own costal cartilages.
- All primary cartilaginous joints are quite immobile and are very strong. The adjacent bone may fracture, but the bone–cartilage interface will not separate.
- They Includes epiphyseal cartilage plates (the union between the epiphysis and the diaphysis of a growing bone) and spheno-occipital and manubrio-sternal synchondroses.
- Secondary cartilaginous joints (Symphysis) have bones are united by hyaline plus fibrocartilage.
- These joints are usually in the midline and are slightly mobile.
- Include pubis symphysis, midline intervertebral joints.
- Symphysis is a union between bones whose articular surfaces are covered with a thin lamina of hyaline cartilage. The hyaline laminae are united by fibrocartilage.
- There may be a cavity in the fibrocartilage, but it is never lined with synovial membrane and it contains only tissue fluid.
- Examples are the pubic symphysis and the joint of the sternal angle (between the manubrium and the body of the sternum).
- An intervertebral disc is part of a secondary cartilaginous joint, but here the cavity in the fibrocartilage contains a gel.
- A limited amount of movement is possible in secondary cartilaginous joints, depending on the amount of fibrous tissue within them. All symphyses occur in the midline of the body.
Types of cartilaginous jointExamplesSynchondrosisSpheno-occipital jointEpiphysio-diaphyseal joint (growing bone)SymphysisMidline intervertebral jointSacrococcygeal joint
Synovial joints are freely mobile joints.
Synovial joints are uniaxial: Plane, hinge and pivot; Biaxial: Condylar and ellipsoid; Multiaxial: Saddle, ball and socket.7
Types of synovial joint | Examples |
|---|---|
Plane |
|
Hinge |
|
Pivot (Trochoid) |
|
Condylar |
|
Ellipsoid |
|
Saddle |
|
Ball and socket |
|
Some authors consider these joints condylar: Atlanto-occipital, wrist (radio-carpal), metacarpo-phalangeal (knuckle).
Some authors consider these joints as modified hinge: Temporo-mandibular, knee joint.
The close and loose-packed positions of joins | ||
Joint | Close-packed position | Loose-packed position |
Shoulder | Abduction + lateral rotation | Semi-abduction |
Ulnohumeral | Extension | Semi-flexion |
Radiohumeral | Semi-flexion + semi-pronation | Extension + supination |
Wrist | Dorsiflexion | Semi-flexion |
2nd–5th metacarpophalangeal | Full flexion | Semi-flexion + ulnar deviation |
Interphalangeal (fingers) | Extension | Semi-flexion |
1st carpometacarpal | Full opposition | Neutral position of thumb |
Hip | Extension + medial rotation | Semi-flexion |
Knee | Full extension | Semi-flexion |
Ankle | Dorsiflexion | Neutral position |
Tarsal joints | Full supination | Semi-pronation |
Metatarsophalangeal | Dorsiflexion | Neutral position |
Interphalangeal (toes) | Dorsiflexion | Semi-flexion |
Intervertebral | Extension | Neutral position |
Primary angular motions | Mechanical analogy | Anatomic examples | |
Hinge joint | Flexion and extension only | Door hinge | Humero-ulnar joint Interphalangeal joint |
Pivot joint | Spinning of one member around a single axis of rotation | Doorknob | Humeroredial joint Atlanto-axial joint |
Ellipsoid joint | Biplanar motion (flexion-extension and abduction-adduction) | Flattened convex ellipsoid paired with a concave trough | Radiocarpal joint |
Ball-and-socket joint | Triplanar motion (flexion-extension, abduction-adduction, and internal-external rotation) | Spheric convex surface paired with a concave cup | Glenohumeral joint Coxofemoral (hip) joint |
Plane joint | Typical motions include slide (translation) or combined slide and rotation | Relatively flat surfaces apposing each other, like a book of a table. | Carpometacarpal joints (digits II to IV) Intercarpal joints Intertarsal joints |
Saddle joint | Biplanar motion; spin between bones is possible but may be limited by interlocking nature of joint | Each member has a reciprocally curved concave and convex surface oriented at right angles to the other, like a horse rider and a saddle | Carpometacarpal joint of the thumb Sternoclavicular joint |
Condyloid joint | Biplanar motion; either flexion-extension and abduction-adduction, or flexion-extension and axial rotation (internal-external rotation) | Mostly spheric convex surface that is enlarged in one dimension like a knuckle; paired with a shallow concave cup | Metacarpophalangeal joint Tibiofemoral (knee) joint |
Note: Metacarpophalangeal joint is generally considered as an ellipsoid synovial joint | |||
Synovial Joints
Figs. 8A and B: An ellipsoid joint (A) is shown as analogous to the radiocarpal joint (wrist) (B) The two axes of rotation are shown by the intersecting pins
Figs. 9A and B: A saddle joint (A) is illustrated as analogous to the carpometacarpal joint of the thumb (B). The saddle in A. Represents the trapezium bone. The rider, if present, would represent the base of the thumb's metacarpal. The two axes of rotation are shown in (B)
- Knee joint is a complex joint (involving more than two bones).
- Femoro-tibial joint structurally resembles a hinge joint, but is considered as a condylar type of synovial joint between two condyles of the femur and tibia. In addition, it includes a saddle joint between the femur and the patella.
ASSESSMENT QUESTIONS
- Knee is which type of joint?a. Synarthrosisb. Symphysisc. Amphiarthrosisd. Diarthrosis
- Joint between epiphysis and diaphysis of a long bone is a type of: (AIIMS 2004)a. Plane Synovial jointb. Fibrous jointc. Symphysisd. Synchondrosis
- Innervated structures of joints are all EXCEPT: (NEET Pattern 2013)a. Synoviumb. Capsulec. Articular cartilaged. Ligaments
- Ear ossicles articulate with each other through which type of joints? (NEET Pattern 2012)a. Synostosisb. Synovialc. Synchondrosisd. Syndesmosis
- Median atlantoaxial joint is: (NEET Pattern 2015)a. Condylarb. Cartilaginousc. Fibrousd. Synovial joint
- Intracapsular articular disc is present in which joint? (NEET Pattern 2012)a. Sternoclavicular jointb. Elbowc. Hip jointd. Knee joint
- What kind of a joint is syndesmosis? (NEET Pattern 2012)a. Fibrousb. Plainc. Pivotd. Cartilaginous
- Vomer ala and sphenoidal rostrum junction is: (NEET Pattern 2013)a. Syndesmosisb. Synostosisc. Schindylesisd. Gomphosis
- Pubic symphysis is which type of joint? (NEET Pattern 2015)a. Synovialb. Fibrousc. Cartilaginousd. None of the above
- What type of joint is the growth plate (AIPG 2010)a. Fibrousb. Primary cartilaginousc. Secondary cartilaginousd. Plane joint
- Manubriosternal joint is: (NEET Pattern 2015)a. Primary cartilaginousb. Secondary cartilaginousc. Synoviald. Ellipsoid
- Inferior tibio-fibular joint is:a. Synchondrosisb. Syndesmosisc. Symphysisd. Schindylesis
- The type of joint between the sacrum and the coccyx is a: (AIPG 2005)a. Symphysisb. Synostosisc. Synchondrosisd. Syndesmosis
- Which of the following is a compound condylar joint? (NEET Pattern 2012)a. Kneeb. TM jointc. Wristd. Elbow
- Which of the following is a synovial joint of the condylar variety? (NEET Pattern 2012)a. First carpometacarpal jointb. Metacarpophalangeal jointc. Interphalangeal jointd. Radiocarpal joint
- Which of the following is the type of joints between malleus and incus?a. Primary cartilaginousb. Secondary cartilaginousc. Saddle synoviald. Ball & socket synovial
- Atlanto-occipital joint is of synovial variety:a. Trochoidb. Ellipsoidc. Condylard. Saddle
ANSWERS AND EXPLANATIONS
- d. Diarthrosis
- Synarthrosis are immovable joints and include the fibrous joints.
- Amphiarthrosis are slight mobile and include the cartilaginous joints
- Diarthrosis are freely mobile joints and include the synovial joints.
- d. Synchondrosis
- Epiphysio-diaphyseal joint is a primary cartilaginous joint – synchondrosis.
- It is found in the growing bone, where the growth plate (hyaline cartilage) connects the epiphysis with the diaphysis, creating a hyaline cartilaginous joint.
- A this site the fate of synchondrosis is synostosis (bony fusion) after the growth plate gets removed and replaced by the bone.
-
- Articular cartilage is devoid of neurovascular bundle.
- b. Synovial
- Malleus-incus joint is a saddle synovial joint and incus -stapes is ball and socket synovial joint.
- d. Synovial joint
- Median atlanto-axial joint is a pivot synovial joint.
- a. Sternoclavicular joint
- Few synovial joints have articular disc is present between articulating bones, e.g. sternoclavicular joint, temporomandibular joint.
- a. Fibrous
- Fibrous joints are three types: sutures, syndesmosis, and gomphoses.
- c. Schindylesis
- Spheno-vomerine joint is a schindylesis suture at the roof of the nasal cavity.
- c. Cartilaginous
- Pubic symphysis is a secondary cartilaginous joint, which is slightly mobile.
- b. Primary cartilaginous
- Growing bones have epiphyseal (growth) plate between the epiphysis and diaphysis, this epphyseo-diaphyseal joint is primary cartilaginous (synchondrosis).
- b. Secondary cartilaginous
- Manubriosternal joint is a symphysis (secondary cartilaginous) joint.
- b. Syndesmosis
- a. Symphysis
- Sacrococcygeal is a secondary cartilaginous (symphysis) joint.
- a. Knee
- Knee joint has more than two bones participating (hence compound joint). It is formed by the lateral and medial femorotibial and the femoropatellar joints.
- It is a compound synovial joint incorporating 2 condylar joints between the condyles of the femur and tibia and one saddle joint between the femur and the patella.
- The TM joint is a condylar joint but it involves only 2 bones (not a compound joint).
- The wrist joint is an ellipsoid synovial joint.
- The elbow joint is a hinge synovial joint.
- b. Metacarpophalangeal joint > d. Radiocarpal joint
- This a wrong question, since Gray's anatomy mentions both the joints under condylar variety.
- Both the joints have condyles with ellipsoid articular surface - are structurally condylar but functionally ellipsoid.
- Some authors mentions metacarpophalangeal as condylar synovial joint only (hence the answer of first preference).
- c. Saddle synovial
- Malleus and incus have saddle synovial joint.
- Incus and stapes have ball & socket synovial joint.
- b. Ellipsoid > c. Condylar
- Functionally it is an ellipsoid synovial joint but structurally it is a condylar synovial joint.
- Head flexion and extension occurs at this joint for the nodding (yes) movement.
Muscles
The orientation of individual skeletal muscle fibres is either parallel or oblique to the line of pull of the whole muscle.
The range of contraction is long with the former arrangement, while the latter provides increased force of contraction. Sartorius is an example of a muscle with parallel fibres.
Muscles with an oblique disposition of fibres fall into several patterns:
- Muscles with parallel fasciculi: These are muscles in which the fasciculi are parallel to the line of pull and have greater degree of movement. These muscles may be:
- Quadrilateral e.g. thyrohyoid
- Strap-like e.g. sternohyoid and sartorius
- Strap-like with tendinous intersections e.g. rectus abdominis
- Fusiform e.g. biceps brachii, digastric
- 11Muscles with oblique fasciculi: When the fasciculi are oblique to the line of pull, the muscle may be triangular, or pennate (feather-like) in the construction. This arrangement makes the muscle more powerful, although the range of movement is reduced. Oblique arrangements are of the following types:
- Triangular e.g. temporalis, adductor longus.
- Unipennate e.g. flexor pollicis longus, extensor digitorum longus
- Bipennate e.g. rectus femoris, flexor hallucis longus
- Multipennate e.g. tibialis anterior, subscapularis, deltoid (acromial fibers]
Common sites of intramuscular injection
Upper arm (Deltoid) |
|
Gluteal region |
|
Thigh (lateral aspect)(vastus lateralis) |
|
Composite or hybrid muscles:
Definition: (a) A muscle having more than one set of muscle fibres (major criteria); (b) A muscle having more than one nerve supply (minor criteria).
Name of muscle | Nerve supply (part of muscle) |
Trapezius |
|
Digastric |
|
Brachialis |
|
Flexor digitorum profundus |
|
Flexor pollicis brevis |
|
Opponens pollicis |
|
Ilio-psoas |
|
Pectineus |
|
Biceps femoris |
|
Adductor magnus |
|
12Some authors give another definition to composite muscle: Composite muscles are those, whose functions are regarded the same in terms of skeletal structure and muscle arrangement condition, as a single muscle model.
- A single muscle itself is considered as a composite muscle, when its different parts work together to perform a particular function and mostly supplied by a single nerve. For example 1)
- Tongue is a composite muscle made up of various components like longitudinal, transverse, horizontal muscles with different parts innervated by a single nerve supply - hypoglossal nerve. 2)
- Quadriceps femoris has four parts, involved in one common activity of knee extension and supplied by a single nerve - femoral nerve.
- Unit concept of muscle: In single-unit smooth muscle, either the whole muscle contracts or the whole muscle relaxes.
- An action potential can be propagated through neighbouring muscle cells due to the presence of many gap junctions between the cells.
- Due to this property single-unit smooth muscle form a syncytium that contracts in a coordinated fashion uterus, gastro-intestinal tract, and the bladder.
In multi-unit smooth muscle, the smooth muscle cells in an organ all behave independently – each cell contract and relaxes on its own.
Single unit type | Multiple unit type |
Digestive tract | Iris |
Urinary tract (includes ureter, bladder) | Trachea and bronchi |
Uterus | Erector pilorum |
Blood vessels (except large elastic arteries) | Large elastic artery |
Ducts deferens |
ASSESSMENT QUESTIONS
- Smallest muscle in the body is: (NEET Pattern 2015)a. Interarytenoidb. Stapediusc. Corrugator supercillid. Superior oblique
- Composite muscles include the following EXCEPT: (AIPG 2008)a. Pectineusb. Adductor magnusc. Rectus femorisd. Biceps femoris
- All are composite muscles EXCEPT: (AIPG 2009)a. Pectineusb. Flexor Carpi ulnarisc. Biceps femorisd. Flexor digitorum profundus
- Muscle having double nerve supply: (PGIC 2015)a. Digastric muscleb. Omohyoid musclec. Trapeziusd. Thyrohyoid musclee. Adductor magnus
- Digastric muscles are the following EXCEPT: (AIPG 2008)a. Occipitofrontalisb. Sternocleidomastoidc. Omohyoidd. Muscular fibres in the ligament of Treitz
- Most common muscle to be congenitally absent is: (AIPG 2009)a. Pectoralis majorb. Teres minorc. Semimembranosusd. Gastrocnemius
- Which among the following is an intra- articular tendon is? (JIPMER 2016)a. Anconeusb. Semitendinosusc. Semimembranosusd. Popliteus
- Which of the following is multipennate muscle? (NEET Pattern 2015)a. FPLb. EPLc. Deltoidd. FHL
- Longest muscle in the body: (NEET Pattern 2012)a. Bicepsb. Tricepsc. Sartoriusd. Quadriceps
- Multi-unit smooth muscle present at all EXCEPT: (NEET Pattern 2012)a. Blood vesselsb. Irisc. Gutd. Ductus deferens
- Single unit smooth muscles are seen in: (NEET Pattern 2012)a. Irisb. Ductus deferensc. Ureterd. Trachea
- Muscle with parallel fibres are all EXCEPT: (AIIMS 2016)a. Sartoriusb. Rectus abdominisc. Sternohyoidd. Tibialis anterior
ANSWERS AND EXPLANATIONS
- b. Stapedius
- The smallest skeletal muscle in the body is stapedius.
- The smallest muscle in the body is arrector pilorum, a smooth muscle in the skin for erection of hair.
-
- Muscles like adductor magnus, pectineus, biceps femoris are called as composite muscles as they have more than one set of muscles fibres and more than one motor nerve supply.
- Rectus femoris is supplied by only one nerve – the femoral nerve and is not a composite muscle.
- b. Flexor carpi ulnaris
- Flexor carpi ulnaris is supplied by a single nerve and is not a composite/hybrid muscle.
- Composite/hybrid muscles have more than one set of fibres and are supplied usually by different nerves for different set of fibres.
- Pectineus has anterior set of fibres supplied by the femoral nerve, whereas, posterior set of fibres may be supplied by the obturator nerve.
- Long head of biceps femoris is supplied by the tibial part of sciatic nerve, and the short head is supplied by the common peroneal nerve. This reflects the composite derivation from the flexor and extensor musculature.
- Radial half of flexor digitorum profundus is supplied by the median nerve and the ulnar half is supplied by the ulnar nerve.
- a. Digastric muscle; c. Trapezius; e. Adductor magnus
- Anterior belly of digastric is supplied by trigeminal nerve and posterior belly by facial nerve.
- Spinal accessory nerve give motor fibres to trapezius muscle, whereas ventral rami of C3,4 are proprioceptive.
- Adductor magnus ischial part is supplied by tibial part of sciatic nerve and adductor part by obturator nerve.
- Inferior belly of the omohyoid is innervated by C1-C3 and the superior belly C1 fibres of ansa cervicalis.
- Thyrohyoid muscle is innervated by C1 fibers travelling with the hypoglossal nerve.
- b. Sternocleidomastoid
- Sternocleidomastoid is a muscle with two heads and one belly, like the biceps brachii.
- Ligament of Treitz is a digastric muscle with a skeletal muscle belly, which arises from the left crus of diaphragm and a smooth muscle belly which arises from the duodeno-jejunal junction.
- It has an intermediate tendon attaching to the connective tissue around the celiac trunk of aorta.
- a. Pectoralis major
- Pectoralis major and minor are the most common congenitally absent muscles.
- Agenesis is often partial and may be a part of the syndrome – Poland syndrome.
- d. Popliteus
- Popliteus has intracapsular origin from the lateral femoral epicondyle. It inserts on the posterior surface of the tibia, just proximal to the soleal line.
- c. Deltoid
- Multipennate muscle has the fiber bundles converge to several tendons.
- c. Sartorius
- The longest muscle of body is sartorius muscle.
- c. Gut
- Gut comes under single-unit smooth muscle, where the whole muscle contracts or the whole muscle relaxes.
- Examples are uterus, gastro-intestinal tract, and the bladder.
- c. Ureter
- In single-unit smooth muscle, either the whole muscle contracts or the whole muscle relaxes.
- d. Tibialis anterior
- The individual fibers of a muscle are arranged either parallel or oblique to the long axis of the muscle.
- Tibialis anterior muscle is a multipennate muscle with oblique fibres.
- Muscles with parallel fasciculi: These are muscles in which the fasciculi are parallel to the line of pull and have greater degree of movement. Few examples are:
- Strap-like e.g. sternohyoid and sartorius
- Strap-like with tendinous intersections e.g. rectus abdominis
Structures Associated with Muscles
Raphe is the line of union of symmetrical structures by a fibrous or tendinous band such as the pterygomandibular, pharyngeal, and scrotal raphes.
Ligaments
Ligaments are fibrous bands that connect bones to bones or cartilage or are folds of peritoneum serving to support visceral structures.
- They are composed of dense connective tissue, mainly collagen fibres, the direction of the fibres being related to the stresses which they undergo.
- In general ligaments are unstretchable, unless subjected to prolonged strain. A few ligaments, such as the ligamenta flava between vertebral lamina and the ligamentum nuchae at the back of the neck, are made of elastic fibres, which enables them to stretch and regain their original length thereafter.
Tendons
Tendons are fibrous bands of dense connective tissue that connect muscles to bones or cartilage.
- They are supplied by sensory fibers extending from muscle nerves.
- They have a similar structure to collagenous ligaments, and attach muscle to bone.
- They may be cylindrical, or flattened into sheet-like aponeuroses.
- Tendons have a blood supply from vessels which descend from the muscle belly and anastomose with periosteal vessels at the bony attachment.
Synovial sheaths
Where tendons bear heavily on adjacent structures, and especially where they pass around loops or pulleys of fibrous tissue or bone and change the direction of their pull, they are lubricated by being provided with a synovial sheath.
- The parietal layer of the sheath is attached to the surrounding structures, the visceral layer is fixed to the tendon, and the two layers glide on each other, lubricated by a thin film of synovial fluid secreted by the lining cells of the sheath.
- The visceral and parietal layers join each other at the ends of their extent.
- Usually they do not enclose the tendon cylindrically; it is as though the tendon was pushed into the double layers of the closed sheath from one side. In this way blood vessels can enter the tendon to reinforce the longitudinal anastomosis. In other cases blood vessels perforate the sheath and raise up a synovial fold like a little mesentery—a vinculum—as in the flexor tendons of the digits.
Aponeuroses are flat fibrous sheets or expanded broad tendons that attach to muscles and serve as the means of origin or insertion of a flat muscle.
Retinaculum
- Is a fibrous band that holds a structure in place in the region of joints.
Bursae
- Are fluid-filled flattened sacs of synovial membrane that facilitate movement by minimizing friction.
Synovial tendon sheaths
- Are synovial fluid-filled tubular sacs around muscle tendons that facilitate movement by reducing friction.
Fascia
- Is a fibrous sheet that envelops the body under the skin and invests the muscles and may limit the spread of pus and extravasated fluids such as urine and blood.
Superficial fascia
Is a loose connective tissue between the dermis and the deep (investing) fascia and has a fatty superficial layer (fat, cutaneous vessels, nerves, lymphatics, and glands) and a membranous deep layer.
- The skin is connected to the underlying bones or deep fascia by a layer of loose areolar connective tissue. This layer, usually referred to as superficial fascia, is of variable thickness and fat content.
- Flat sheets of muscles are also present in some regions. These include both skeletal muscles (platysma, palmaris brevis) and smooth muscles (subareolar muscle of the nipple, dartos, corrugator cutis ani).
- The superficial fascia is most distinct on the lower abdominal wall where it differentiates into two layers. Strong connective tissue bands traverse the superficial fascia binding the skin to the underlying aponeurosis of the scalp, palm and sole.
Deep Fascia
- Is a sheet of fibrous tissue that invests the muscles and helps support them by serving as an elastic sheath or stocking.
- Provides origins or insertions for muscles, forms fibrous sheaths or retinacula for tendons, and forms potential pathways for infection or extravasation of fluids.
- The limbs and body wall are wrapped in deep fascia. It varies widely in thickness.
- In the iliotibial tract of the fascia lata, for example, it is very well developed, while over the rectus sheath and external oblique aponeurosis of the abdominal wall, it is so thin as to be scarcely demonstrable and is usually considered to be absent.
- In other parts, such as the face and the ischioanal fossa, it is entirely absent.
- Where deep fascia passes directly over bone it is always anchored firmly to the periosteum and the underlying bone is described as being subcutaneous.
- In the neck, as well as the investing layer of deep fascia, there are other deeper fascial layers enclosing neurovascular structures, glands and muscles. Intermuscular septa are laminae of deep fascia which extend between muscle groups.
- In the neck, as well as the investing layer of deep fascia, there are other deeper fascial layers enclosing neurovascular structures, glands and muscles. Intermuscular septa are laminae of deep fascia which extend between muscle groups.
- Transverse thickenings of deep fascia over tendons, attached at their margins to bones, form retinaculae at the wrists and ankles and fibrous sheaths on the fingers and toes.
Retinacula at the joints
In the vicinity of the joints, the tendons of the muscles of the leg are bound down by localized, band-shaped thickenings of the deep fascia termed retinacula, which collectively serve to prevent bowstringing of the underlying tendons during muscle contraction.15
Portal Venous Circulation
- Portal circulation is a capillary network that lies between two veins. Blood supplying the organ thus passes through two sets of capillaries before it returns to the heart.
- In hepatic portal system blood supplying the abdominal organs passes through two sets of capillaries before it returns to the heart.
- A portal circulation also connects the median eminence and infundibulum of the hypothalamus with the adenohypophysis.
- In the renal glomeruli. The glomerular capillary bed lies between afferent and efferent arterioles and may be considered as a portal circulation, but most of the authors do not mention so (including Gray's anatomy).
ASSESSMENT QUESTION
- NOT true about shunt vessel is: (AIPG 2009)a. It control temperature regulationb. It is direct communication between artery and veinsc. It is under control of local mediatorsd. It is not under autonomic control
ANSWER WITH EXPLANATION
- d. It is not under autonomic control
- Shunt vessels are under the vasoconstrictive action of sympathetic nervous system.
- Under sympathetic control the shunt vessel is able to close completely, diverting blood into the normal pathway.
- Shunt vessels are direct arterio-venous communication between smaller arteries and veins.
Lymphatic System
Lymphatic system is a collection of vessels that function to drain extracellular fluid from tissues of the body and return it to the venous system.
The lymphatic system consists of lymphatic organs, a conducting network of lymphatic vessels, and the circulating lymph.
Primary or central lymphoid organs generate lymphocytes from immature progenitor (stem) cells.
The thymus and the bone marrow constitute the primary lymphoid organs involved in the production and early clonal selection of lymphocyte tissues.
- Bone marrow is responsible for both the creation of T cells and the production and maturation of B cells. From the bone marrow, B lymphocytes immediately join the circulatory system and travel to secondary lymphoid organs in search of pathogens.
- T lymphocytes on the other hand, travel from the bone marrow to the thymus, where they develop further. Mature T cells join B cells in search of pathogens. The other 95% of T cells begin a process of apoptosis, a form of programmed cell death.
Secondary or peripheral lymphoid organs, which include lymph nodes and the spleen, maintain mature naive lymphocytes and initiate an adaptive immune response.
- The peripheral lymphoid organs are the sites of lymphocyte activation by antigens. Activation leads to clonal expansion and affinity maturation. Mature lymphocytes recirculate between the blood and the peripheral lymphoid organs until they encounter their specific antigen.
- Secondary lymphoid tissue provides the environment for the foreign or altered native molecules (antigens) to interact with the lymphocytes. It is exemplified by the lymph nodes, and the lymphoid follicles in tonsils, Peyer's patches, spleen, adenoids, skin, etc. That are associated with the mucosa-associated lymphoid tissue (MALT).
- In the gastrointestinal wall the vermiform appendix has mucosa resembling that of the colon, but here it is heavily infiltrated with lymphocytes.
Tertiary lymphoid organs (TLOs) are included postnatally in non-lmyphoid tissue such as those affected by chronic infection, autoimmune disease, and chronic allograft rejection, and also in cancer tissue.
- They have a structure similar to that of lymph nodes or Peyer's patches, including T cell zones, B cell follicles, and high endothelial venules (HEV) without encapsulation.
17All regions of the body possess lymphatic drainage except for the brain and spinal cord. Right upper quadrant of the body drains the lymphatics into the right lymphatic duct and rest of the body drains into thoracic duct.
The confluence of lymph trunks receives lymph from fourma in lymphatic trunks: The right and left lumbar lymph trunks and the right and left intestinal lymph trunks.
In a small percentage of population this abdominal confluence of lymph trunks is represented as a dilated sac called the cisterna chyli. It is present in the abdomen at L-1, 2 vertebral levels.
Thoracic Duct begins in the abdomen at T-12 vertebral level as the continuation of cisterna chyli.
- It is usually beaded because of its numerous valves and often forms double or triple ducts.
- It drains the body below diaphragm (lower limbs, pelvis, abdomen) and left half of the body above diaphragm (thorax, upper limb and the head and neck).
- Thoracic duct passes through the aortic hiatus in the diaphragm and ascends through the posterior mediastinum between the aorta and the azygos vein.
- At T-5 vertebral level it deviates to left side of midline and keep ascending up to pass the thoracic inlet. It arches laterally over the apex of the left pleura and between the left carotid sheath in front and the vertebral artery behind, runs behind the left internal jugular vein, and eventually empties into the left venous angle — junction of the left internal jugular and subclavian veins (Beginning right brachiocephalic vein).
Tributaries of thoracic duct:
- Bilateral (right and left) descending thoracic lymph trunks, which convey lymph from the lower intercostal spaces (6 to 11).
- Left upper intercostal lymph trunks, which convey lymph from the left upper intercostal spaces (1 to 5).
- Mediastinal lymph trunks
- Left subclavian lymph trunk
- Left jugular lymph trunk
- Left bronchomediastinal lymph trunk
Fig. 15A and B: (A) Thoracic duct and right lymphatic duct. (B) Formation, course and termination of thoracic duct
Right lymphatic duct is a short vessel that drains the right upper half of the body above diaphragm.
- It begins as a convergence of the right sided lymphatic vessels (subclavian lymph trunk, jugular lymph trunk, and bronchomediastinal lymph trunk).
- It drains into the right venous angle - junction of the right internal jugular and subclavian veins (Beginning of left brachiocephalic vein).
- Right lymphatic duct drains right side of the head and neck, upper limb, thorax (including breast and lung) and superficial thoracoabdominal wall (above umbilicus).
Fig. 16: Summary diagram of specific lymphatic drainage. Arrow indicate direction of lymph flow. Right side of body above diaphragm – Shaded boxed area (light brown), lymph drainage into the right lymphatic duct; Rest of the body lymph drain into the thoracic duct.
ASSESSMENT QUESTIONS
- Thoracic duct does NOT drain: (NEET Pattern 2013)a. Right upper part of bodyb. Left upper part of bodyc. Right lower part of bodyd. Left lower part of body
- All are true about thoracic duct EXCEPT:a. Begins as continuation of cisterna chyli (NEET Pattern 2014)b. Largest lymphatic vesselc. Passes through the esophageal openingd. Ends into junction between left subclavian and internal jugular vein
-
a. Subclavian veinb. Internal jugular veinc. Right brachiocephalic veind. Left brachiocephalic vein
- The thoracic duct receives tributaries from all of the following EXCEPT: (AIIMS 2008)a. Bilateral ascending lumbar trunkb. Bilateral descending thoracic trunkc. Left upper intercostal ductd. Right bronchomediastinal lymphatic trunk
- All is true about Pecquet duct EXCEPT:a. Begins at level of T12b. Enters thorax through aortic openingc. Crosses from right to left at level of T8d. Passes the superior aperture of thoraxe. Passes in posterior and superior mediastinum
ANSWERS AND EXPLANATIONS
- a. Right upper part of body
- Right upper quadrant of the body drains the lymphatics into the right lymphatic duct and rest of the body drains into thoracic duct.
- c. Passes through the esophageal opening
- Thoracic duct passes through the aortic hiatus in front of the T 12 vertebra, lying on the right side of aorta.
- d. Left brachiocephalic vein
- Thoracic duct opens into the left venous (jugulo-subclavian) angle, at the beginning of left brachio-cephalic vein.
- d. Right bronchomediastinal lymphatic trunk
- Right broncho-mediastinal lymphatic trunk drains into right lymphatic duct (not thoracic duct).
- Theme: Right half of the body above diaphragm (right superior quadrant) drains into the right lymphatic duct.
- Right lymphatic duct receives the lymphatic drainage from the right half of the head & neck (Jugular lymphatic trunk); right upper limb (right subclavian lymphatic trunk) and the right thoracic cavity (right broncho-mediastinal lymphatic trunk and the right upper intercostal ducts).
- Thoracic duct drains the body below the diaphragm and also the remaining left superior quadrant of the body.
- Hence, it receives the left sided jugular, subclavian and broncho-mediastinal lymphatic trunks.
- It also receives left upper intercostal ducts whereas, right upper intercostal ducts empty into the right lymphatic duct.
- Thoracic duct receives three major lymphatic vessels at its commencement: Bilateral ascending lumbar ducts; Bilateral descending thoracic ducts and Intestinal lymphatic trunks.
- Bilateral descending thoracic ducts drain the lower 6 intercostal spaces (embryologically this region comes below diaphragm) and empty into the thoracic duct.
- As noted above upper 6 intercostal spaces on the right drain into the right lymphatic duct and left upper intercostals into thoracic duct accordingly.
- Important: Right thoracic duct not only receives the lymphatics of right lung (lungs lie above diaphragm) but also lower lobe of left lung ! Upper lobe of left lung drains into the thoracic duct only.
- Externally umbilicus (in place of diaphragm) is taken to be the watershed line i.e., skin above the umbilicus on right side of the body drains into the right lymphatic duct.
- c. Crosses from right to left at level of T8
- Thoracic (Pecquet) duct crosses from right to left at level of T5 vertebra.
Miscellaneous
ASSESSMENT QUESTION
- Embalming solution constituents are all EXCEPT: (AIIMS 2008)a. Ethanolb. Phenolc. Glycerined. Formalin
ANSWER WITH EXPLANATIONS
- a. Ethanol
- Ethanol is a preservative and can be used for embalming but is not the usual content of embalming fluid/solution. In its place methanol is used, which is cheaper and more toxic to bacteria than ethanol.
- Embalming is the process of treatment of the dead body with antiseptics and preservatives to prevent putrefaction.
- Preservative is the substance added to destroy or inhibit the growth of micro-organisms. It alters enzymes and lysins of the body and arrest decomposition — fixing the specimen in such a way that it retains its original structure with minimal alteration.
- Formalin is the most commonly used fixative/ preservative and less commonly used are – Ethanol/ Phenol.
- Phenol is a powerful Fungicide.
- Glycerine is used in the embalming fluid as a hygroscopic/humectant/wetting agent and decreases the loss of water of the preserved structures (maintains hydration). But it is not the actual preservative by definition.
- Wetting agents lower the surface tension of water and facilitate penetration and distribution of embalming fluids through the vascular beds into the tissues.